
Continuous glucose monitoring provides a new, less invasive method for evaluating diabetes risk.
Fluctuations in blood glucose are more than just daily energy swings—they may hold the key to identifying diabetes risk earlier and more easily, without the need for needle-based tests.
Researchers at the University of Tokyo have developed a simple, noninvasive method for evaluating blood glucose regulation, a crucial factor in determining diabetes risk. Using data from continuous glucose monitoring (CGM) devices, their approach could significantly improve early detection and risk prediction without depending on blood draws or costly procedures.
The study is published in Communications Medicine.
Current tests miss early warning signs
Diabetes, often described as a “silent epidemic,” continues to rise globally, posing major health and economic challenges. Detecting impaired glucose regulation early, before it progresses to Type 2 diabetes, is critical for prevention. However, standard tests often miss these early warning signs, since they rely on intermittent blood samples rather than capturing real-time glucose patterns.
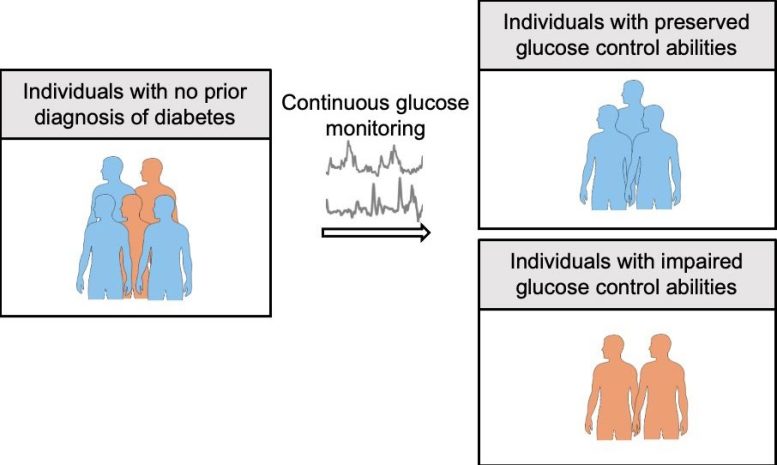
“Traditional diabetes tests, while useful, do not capture the dynamic nature of glucose regulation under physiological conditions,” said Shinya Kuroda, a professor at the University of Tokyo’s Graduate School of Science and co-author of the current study.
Testing CGM accuracy with advanced analysis
To find a more practical alternative, the team turned to CGM, a wearable technology that continuously tracks glucose levels in real time, providing a clearer picture of blood glucose fluctuations in everyday life. Their goal was to identify a CGM-based method for estimating glucose handling capacity, which maintains stable levels, without invasive procedures.
The team analyzed 64 individuals without a prior diabetes diagnosis, using a CGM device, oral glucose tolerance tests (OGTT), and clamp tests that are used to assess insulin sensitivity and glucose metabolism. They then validated their findings with an independent dataset and mathematical simulations.
CGM algorithm detects hidden glucose issues
Their analysis showed that AC_Var, a measure of glucose-level fluctuations, strongly correlates with the disposition index, a well-established predictor of future diabetes risk. Moreover, the researchers’ model, which combines AC_Var with glucose standard deviation, outperformed traditional diabetes markers — such as fasting blood glucose, HbA1c and OGTT results — in predicting the disposition index.
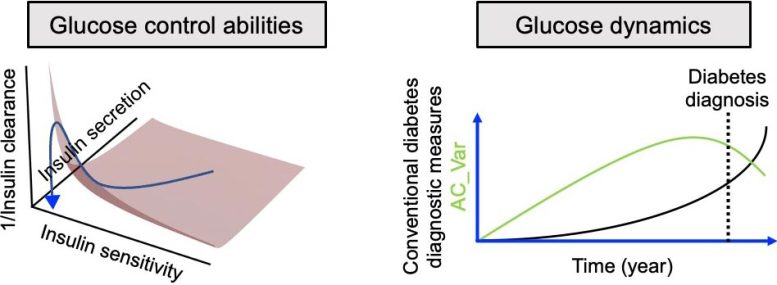
“By analyzing CGM data with our new algorithm, we identified individuals with impaired glycemic control — even when standard diagnostic tests classified them as ‘normal,’” said Kuroda. “This means we can potentially detect issues much earlier, creating an opportunity for preventive interventions before diabetes is diagnosed.”
The team also showed that the method was more accurate than conventional diagnostic indicators in predicting diabetes complications such as coronary artery disease. To facilitate broader access to this approach, the research team has developed a web application that allows individuals and health care providers to easily calculate these CGM-based indices.
“Our ultimate goal is to provide a practical, accessible tool for widespread diabetes screening,” Kuroda said. “By enabling early detection of glucose regulation abnormalities, we hope to prevent or delay disease onset and reduce long-term complications.”
Reference: “Improved detection of decreased glucose handling capacities via continuous glucose monitoring-derived indices” by Hikaru Sugimoto, Ken-ichi Hironaka, Tomoaki Nakamura, Tomoko Yamada, Hiroshi Miura, Natsu Otowa-Suematsu, Masashi Fujii, Yushi Hirota, Kazuhiko Sakaguchi, Wataru Ogawa and Shinya Kuroda, 22 April 2025, Communications Medicine.
DOI: 10.1038/s43856-025-00819-5
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.
1 Comment
You gotta love the sales pitch title: “This Device Could Spot Diabetes Before It Starts, No Needles Required”. Spotting something before it starts is a real trick. If you spotted it, it already started. If it didn’t already start, then you are not spotting it, but are guessing it will start.
This study continually monitored the blood glucose level, but ignored all the stresses and demands of life that alter blood sugar levels throughout the day and night. Fluctuations in glucose level is normal. From the study, “Recent studies have revealed substantial heterogeneity in glucose fluctuation patterns, even among individuals classified as having normal glucose tolerance (NGT) according to conventional criteria.”
There was no control group of people who did not wear their device that detects glucose. Wearing the device could affect sugar levels since it raises expectations and concerns in the people wearing it.
Attempts to identify a disease before it exists is over-medicalization, and can result in unnecessary “preventive” treatments. Predictions of the future are best left to soothsayers and mystics.