
Parkinson’s Disease May Be Detected in Its Early Stages Through the Use of Special Brain Scans
Parkinson’s disease is a debilitating brain condition that worsens with time and affects sufferers’ ability to walk and even talk. It’s complex to diagnose, and in the early stages – impossible.
Most of us are acquainted with a method known as MRI, which is often used to visualize brain structure. However, it is currently only used to rule out other potential diagnoses since it is not sensitive enough to show the biological changes that occur in Parkinson’s patients’ brains.
Advancing Diagnosis with Quantitative MRI (qMRI)
Researchers at the Hebrew University of Jerusalem (HU), under the direction of Professor Aviv Mezer, came to the conclusion that by modifying a related method known as quantitative MRI (qMRI), it could be possible to reveal the cellular changes in Parkinson’s. With the use of their technique, they were able to examine the microstructures of the striatum, an area of the deep brain that is known to degenerate as Parkinson’s disease progresses.
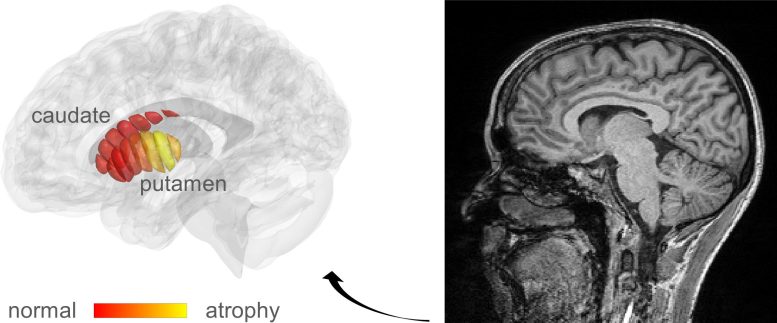
Using a new method of analysis, developed by Mezer’s doctoral student, Elior Drori, biological changes in the cellar tissue of the striatum were clearly revealed. Moreover, they were able to demonstrate that these changes were associated with the early stages of Parkinson’s and patients’ movement dysfunction. Their findings were recently published in the prestigious journal Science Advances.
Sensitivity Beyond Standard MRI Techniques
qMRI achieves its sensitivity by taking several MRI images using different excitation energies – rather than taking the same photograph in different colors of lighting. The HU researchers were able to use their qMRI analysis to reveal changes in the tissue structure within distinct regions of the striatum. The structural sensitivity of these measurements could only have been previously achieved in laboratories examining the brain cells of patients post-mortem. Not an ideal situation for detecting early disease or monitoring the efficacy of a drug!
“When you don’t have measurements, you don’t know what is normal and what is abnormal brain structure, and what is changing during the progress of the disease,” explained Mezer. The new information will facilitate early diagnosis of the disease and provide “markers” for monitoring the efficacy of future drug therapies.
“What we have discovered,” he continued “is the tip of the iceberg.” It is a technique that they will now extend to investigate microstructural changes in other regions of the brain. Furthermore, the team is now developing qMRI into a tool that can be used in a clinical setting. Mezer anticipates that is about 3-5 years down the line.
Drori further suggests that this type of analysis will enable the identification of subgroups within the population suffering from Parkinson’s disease – some of whom may respond differently to some drugs than others. Ultimately, he sees this analysis as “leading to personalized treatment, allowing future discoveries of drug with each person receiving the most appropriate drug.”
Reference: “Mapping microstructural gradients of the human striatum in normal aging and Parkinson’s disease” by Elior Drori, Shai Berman and Aviv A. Mezer, 15 July 2022, Science Advances.
DOI: 10.1126/sciadv.abm1971
The study was funded by the Israel Science Foundation.
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.