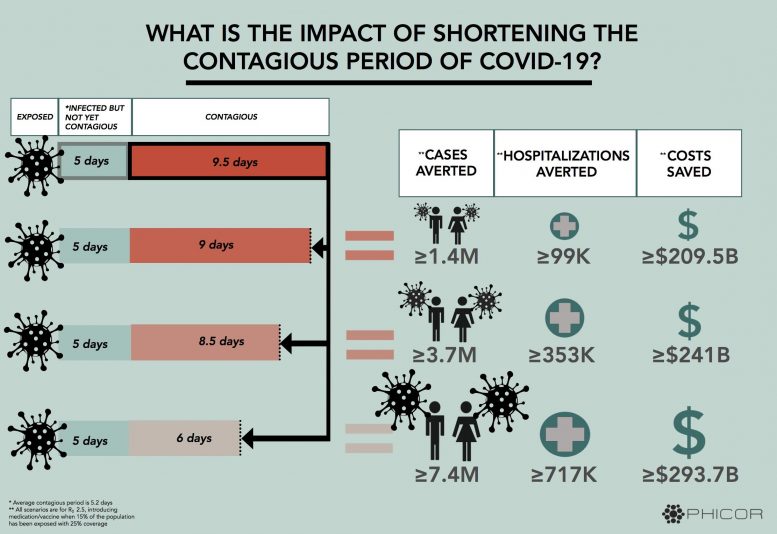
Simulations highlight potential value of developing ways to reduce how long someone is contagious.
A new computational analysis suggests that a vaccine or medication that could shorten the infectious period of COVID-19 may potentially prevent millions of cases and save billions of dollars. The study was led by Bruce Lee along with colleagues in the Public Health Informatics, Computational, and Operations Research (PHICOR) team headquartered at the CUNY Graduate School of Public Health and Health Policy and the Lundquist Research Institute at Harbor-UCLA Medical Center, and publishes in the open-access journal PLOS Computational Biology.
Looking Beyond Prevention and Cure
While much of the public conversation surrounding COVID-19 vaccines and medications has focused on preventing or curing the infection, the vaccines and medications that may emerge could have subtler effects. Those that can’t necessarily prevent or cure may still reduce how long someone is contagious.
To clarify the potential value of shortening the infectious period, Lee and colleagues created a computational model that simulates the spread of SARS-CoV-2, the virus that causes COVID-19. They used the model to explore how a vaccine or medication that can reduce the contagious period might alleviate the clinical and economic impact of the disease.
The simulations suggest that reducing the contagious period by half a day could avert up to 1.4 million cases and over 99,000 hospitalizations, saving $209.5 billion in direct medical and indirect costs — even if only a quarter of people with symptoms were treated — and incorporating conservative estimates of how contagious the virus may be. Under the same circumstances, cutting the contagious period by 3.5 days could avert up to 7.4 million cases. Expanding such treatment to 75 percent of everyone infected could avert 29.7 million cases and save $856 billion.
These findings could help guide research and investments into development of vaccines or medications that reduce the infectious period of SARS-CoV-2. They could also help government agencies plan rollout of such products and provide cost insights to guide reimbursement policies for third-party payers.
Small Changes, Big Difference in Pandemic Control
“There may be a tendency to overlook vaccines and other treatments that don’t prevent a COVID-19 infection or cure disease,” says Lee. “But this study showed that even relatively small changes in how long people are contagious can significantly affect the transmission and spread of the virus and thus save billions of dollars and avert millions of new cases.”
“This study shows that vaccine and medication development efforts for COVID-19 should focus on the impact to actually help curb the spread of the COVID-19 pandemic, not just benefits of a single patient,” says James McKinnell, a co-author of the study. “Widespread treatment, in combination with other prevention efforts, could prove to be the tipping point.”
Reference: “The value of decreasing the duration of the infectious period of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) infection” by Bruce Y. Lee, Sarah M. Bartsch, Marie C. Ferguson, Patrick T. Wedlock, Kelly J. O’Shea, Sheryl S. Siegmund, Sarah N. Cox and James A. McKinnell, 7 January 2021, PLOS Computational Biology.
DOI:
Funding: This work was supported in part by City University of New York (CUNY) Graduate School of Public Health and Health Policy (BYL, SMB, MCF, PTW, KJO, SSS, SNC), the National Institute of General Medical Sciences (NIGMS) as part of the Models of Infectious Disease Agent Study (MIDAS) network under grant 1 R01 GM127512-01A1 (BYL, SMB, MCF, PTW, KJO, SSS, SNC). It was also supported by the Agency for Healthcare Research and Quality (AHRQ) via grant R01HS023317 (BYL, SMB, MCF, PTW, KJO, SSS, SNC), United States Agency for International Development (USAID) under agreement number AID-OAA-A-15-00064 (BYL, SMB, MCF, PTW, KJO, SSS, SNC), and the Eunice Kennedy Shriver National Institute of Child Health and Human Development (NICHD) via grant U01HD086861(BYL, SMB, MCF, PTW, KJO, SSS, SNC), and 5R01HD086013-02(BYL, SMB, MCF, PTW, KJO, SSS, SNC). The funders had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript. The authors of this manuscript are responsible for its content, including data analysis. Statements in the manuscript do not necessarily represent the official views of, or imply endorsement by, National Institute of Health, AHRQ or HHS.
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.