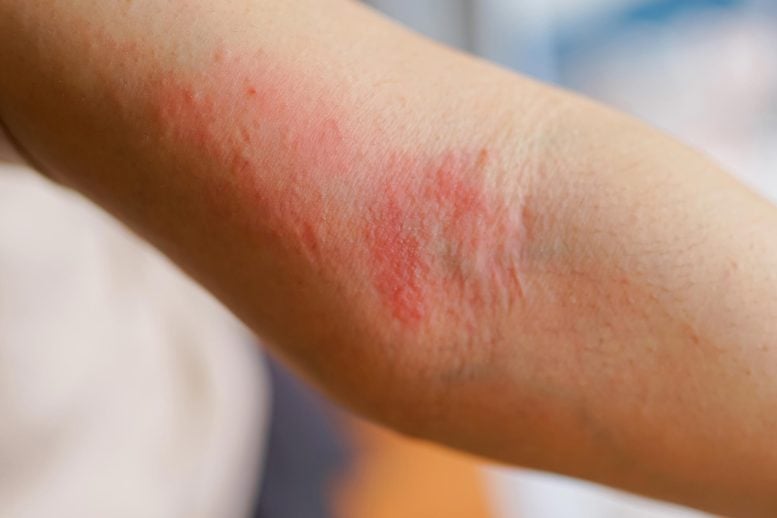
A newly identified brain–immune connection suggests stress may directly amplify skin inflammation through targeted cellular signaling.
Psychological stress has long been blamed for making eczema worse, but the biological link has been hard to pin down. New research now traces that connection to a brain-to-skin signaling route that appears to intensify inflammation by directing nerve activity toward immune cells in the skin. The findings suggest that stress is not just a trigger that people report anecdotally. It may be part of the disease process itself.
If the same stress-linked pathway can be disrupted, either through better stress management or treatments that block the underlying signals, doctors may have another way to reduce flare-ups alongside standard eczema therapies.
“[The authors] offer a mechanistic explanation for the well-documented but poorly understood link between stress and atopic dermatitis flare-ups,” write Nicolas Gaudenzio and Lillan Basso in a related Perspective. “Research into the existence of similar mechanisms in other stress-sensitive inflammatory diseases, such as psoriasis or inflammatory bowel disease, is also needed,” they say.
The Neuroimmune Link in Eczema
Atopic dermatitis, the most common form of eczema, is more than a surface rash. It involves a disrupted skin barrier, chronic inflammation, and intense itching that can feed a damaging cycle of scratching, skin injury, and worsening symptoms. Stress is already known to aggravate that loop by altering immune function, weakening the skin barrier, and amplifying itch.
The skin is especially vulnerable to these effects because it is packed with both nerve endings and immune cells. That makes it one of the body’s most active sites of communication between the nervous system and the immune system. Even so, the exact chain of events connecting psychological stress to immune flare-ups in eczema has remained unclear.
One major suspect has been the eosinophil, an immune cell closely associated with allergic inflammation and severe dermatitis. Eosinophils can release toxic granule proteins and inflammatory molecules that intensify skin damage. What researchers did not fully understand was how stress-related nerve signals draw these cells into the skin and switch them into an inflammatory state.
Investigating Stress Pathways
To investigate, Jiahe Tian and colleagues analyzed clinical data from 51 patients with atopic dermatitis and used mouse models to study how stress affects inflammation in the skin. They found that higher stress was associated with greater eosinophil accumulation in patient skin and identified a subset of prodynorphin-positive (Pdyn+) noradrenergic sympathetic neurons that innervate hairy skin.
Further experiments showed that these neurons relay stress signals from the brain to the skin, where they worsen inflammation in an eosinophil-dependent manner. The neurons recruited eosinophils through the CCL11-CCR3 signaling pathway and activated them through the adrenergic receptor beta2 (Adrb2). Removing either the neurons or eosinophils reduced stress-induced inflammation, while activating the neurons increased it.
The findings suggest that peripheral sympathetic nerves, rather than the hypothalamus-pituitary-adrenal axis, play a central role in this stress response. They also point to stress-induced eosinophilia and the Pdyn+ sympathetic neuron-eosinophil interface as potential therapeutic targets in atopic dermatitis.
Reference: “A sympathetic-eosinophil axis orchestrates psychological stress to exacerbate skin inflammation” by Jiahe Tian, Yudian Cao, Yilei Li, Junlong Sun, Cheng Zhan, Wei Ni, Yongjun Zheng, Yanqing Wang and Shenbin Liu, 19 March 2026, Science.
DOI: 10.1126/science.adv5974
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.
1 Comment
So, should we be looking at the home life of children with eczema for neglect and abuse, physical and emotional and psychological? Could eczema be a symptom of stress from abuse and/or neglect? I have eczema now at 55 and it seems mostly triggered by peanuts and cashews and maybe other nuts and a few other things, and my stress is pretty much constant. But I had eczema when I was a kid, and I was physically and emotionally neglected and psychologically abused by my parents, mostly my mother.
I mean, if you look up photos of eczema, a lot of them are of children and babies. Kids that young should not be having that much stress in their lives. Something is wrong there.