
The transition to electronic health records (EHRs) was supposed to improve the quality and efficiency of healthcare for doctors and patients alike — but these technologies get an “F” rating for usability from health care professionals, and may be contributing to high rates of professional burnout, according to a new Yale-led study.
By contrast, Google’s search engine earned an “A” and ATMs a “B” in similar but separate studies. Like EHRs, the spreadsheet software Excel got an “F.”
“A Google search is easy,” said lead author Edward R. Melnick, assistant professor of emergency medicine and director of the Clinical Informatics Fellowship at Yale. “There’s not a lot of learning or memorization; it’s not very error-prone. Excel, on the other hand, is a super-powerful platform, but you really have to study how to use it. EHRs mimic that.”
Published in the journal Mayo Clinic Proceedings, the new study was a joint effort of researchers at Stanford, Mayo, and the American Medical Association (AMA).
There are various EHR systems that hospitals and other medical clinics use to digitally manage patient information. These systems replace hard-copy files, storing clinical data, such as medications, medical history, lab and radiology reports, and physician notes. They were developed to improve patient care by making health information easy for healthcare providers to access and share, reducing medical errors.
But the rapid rollout of EHRs following the Health Information Technology for Economic and Clinical Health Act of 2009, which pumped $27 billion of federal incentives into the adoption of EHRs in the U.S., forced doctors to adapt quickly to often complex systems, leading to increasing frustration.
The study notes that physicians spend one to two hours on EHRs and other deskwork for every hour spent with patients, and an additional one to two hours daily of personal time on EHR-related activities.
“As recently as 10 years ago, physicians were still scribbling notes,” Melnick said. “Now, there’s a ton of structured data entry, which means that physicians have to check a lot of boxes. Often this structured data does very little to improve care; instead, it’s used for billing. And looking for communication from another doctor or a specific test result in a patient’s chart can be like trying to find a needle in a haystack. The boxes may have been checked, but the patient’s story and information have been lost in the process.”
Melnick’s study zeroed in on the effect of EHRs in physician burnout.
“And that will not only mean less paper-pushing and lower administrative costs, saving taxpayers billion of dollars, it will also mean all of you physicians will have an easier time doing your jobs.” — President Barrack Obama referring to electronic health records while selling his health plan to doctors on June 15, 2009
The AMA, along with researchers at Mayo and Stanford, surveys over 5,000 physicians every three years on topics related to burnout. Most recently, the burnout rate was found to be 43.9% — a drop from 54.4% in 2014, but still worryingly high, researchers said. The same survey found that burnout for the general U.S. population was 28.6%.
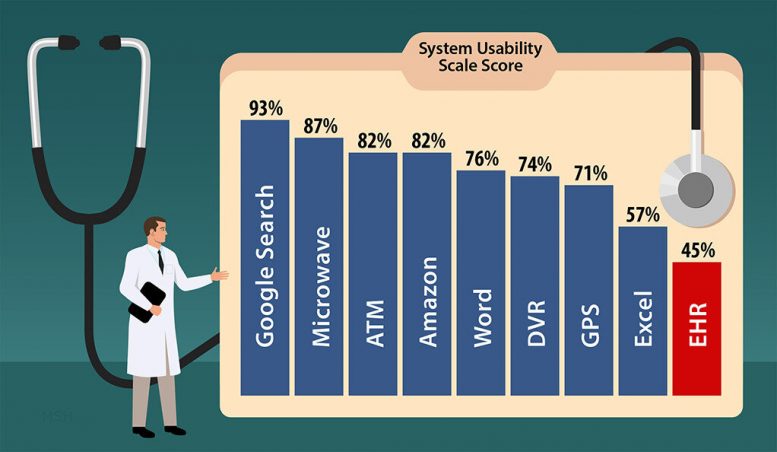
One quarter of the respondents were also asked to rate their EHR’s usability by applying a measure, System Usability Scale (SUS), that has been used in over 1,300 other usability studies in various industries.
Users in other studies ranked Google’s search engine an “A.” Microwave ovens, ATMs, and Amazon got “Bs.” Microsoft Word, DVRs, and GPSes got “Cs.” Microsoft Excel, with its steep learning curve, got an “F.”
In Melnick’s study, EHRs came in last, with a score of 45 — an even lower “F” score than Excel’s 57.
And EHR usability ratings correlated highly with burnout — the lower physicians rated their EHR, the higher the likelihood that they also reported symptoms of burnout.
The study found that certain physician specialties rated their EHRs especially poorly — among them, dermatology, orthopedic surgery, and general surgery.
Conversely, specialties with the highest SUS scores included anesthesiology, general pediatrics, and pediatric subspecialties.
The lower physicians rated their EHR, the higher the likelihood that they also reported symptoms of burnout.
Demographic factors like age and location mattered, too. Older physicians found EHRs less usable, and doctors working in veterans’ hospitals rated their EHR higher than physicians in private practice or academic medical centers.
By benchmarking physicians’ feelings about EHRs, Melnick said, it will be possible to track the impact of technology improvements on usability and burnout.
“We’re trying to improve and standardize EHRs,” Melnick said. “The goal is that with future work, we won’t have to ask doctors how they feel about the EHR or even how burned out they are, but that we can see how doctors are interfacing with the EHR and, when it improves, we can see that improvement.”
Reference: “The Association Between Perceived Electronic Health Record Usability and Professional Burnout Among US Physicians” by Edward R. Melnick, MD, MHS; Liselotte N. Dyrbye, MD, MHPE; Christine A. Sinsky, MD; Mickey Trockel, MD, Ph.D.; Colin P. West, MD, Ph.D.; Laurence Nedelec, Ph.D.; Michael A. Tutty, Ph.D. and Tait Shanafelt, MD, 14 November 2019, Mayo Clinic Proceedings.
DOI: 10.1016/j.mayocp.2019.09.024
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.
14 Comments
I retired early. Found that many duties were checked as being done were NOT. Too many labs that were reasonable under patient diagnosis would be reading red alert and demanding action before any further info could be reviewed. Absurd programming.
Baloney!
EHR and other digital advances in healthcare have prolonged my career by 20 years.
Wow. Physicians in academic medicine finally having to do real work declare EHRs as terrible. What a big surprise.
If doctors respected the IT staffs of their organizations as much as they expect to be respected for they know,many of those kludges, aka medical information systems, would have never been purchased in the condition that they (still) in ten years after they were introduced.
That there is no standard for data interchange, industry GUI for doctors and patients,could have been predicted from an industry that hasn’t completely embraced outcome based medicine, and resists accountability.
As someone who works in Healthcare I don’t think we should be baseing a survey on a population that will cancel an entire days worth of patients, just because they have to use a wired (vs wireless) mouse.
I wouldn’t go to a doctor that’s too backward to use EMR systems. Must have gotten his/her medical training in the 1940’s. Also the HITECH Act requirements make structured data that is useful for research. Evidence-based medicine results in better patient outcomes. Learn for goodness sake.
I dont think you can pin this on Obama. Bush started all of it when he signed ARRA and established Meaningful Use.
That there is no standard for data interchange, industry GUI for doctors and patients,could have been predicted from an industry that hasn’t completely embraced outcome based medicine, and resists accountability.
Physicians in academic medicine finally having to do real work declare EHRs as terrible
behtarin gheimat tour kish dar website azhans arshin parvaz
Physicians in academic medicine finally having to do real work declare EHRs as terrible
Best
Excellent …