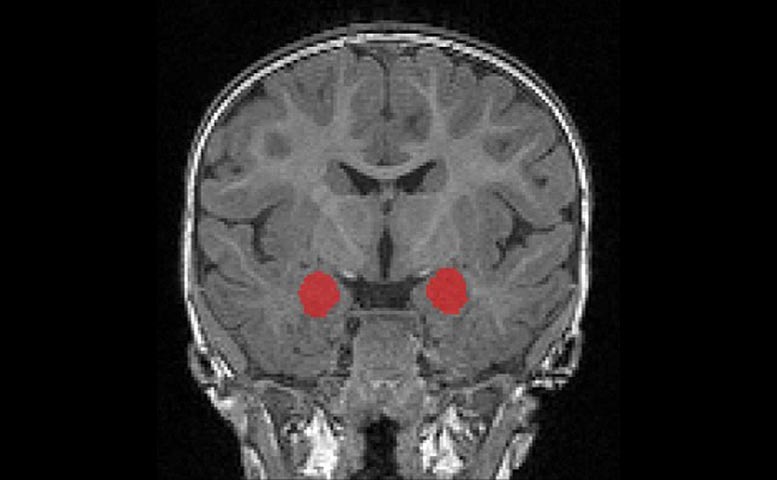
Research led by Mark Shen, PhD, Heather Hazlett , PhD, and Joseph Piven, MD, from UNC-Chapel Hill is the first to demonstrate overgrowth of the amygdala in the first year of life, before babies show most of the behavioral symptoms that later consolidate into a diagnosis of autism. This overgrowth may be unique to autism, as babies with fragile X syndrome show a different brain growth pattern.
The amygdala is a small structure deep in the brain important for interpreting the social and emotional meaning of sensory input – from recognizing emotion in faces to interpreting fearful images that inform us about potential dangers in our surroundings. Historically the amygdala has been thought to play a prominent role in the difficulties with social behavior that are central to autism.
Researchers have long known the amygdala is abnormally large in school-age children with autism, but it was unknown precisely when that enlargement occurs. Now, for the first time, researchers from the Infant Brain Imaging Study (IBIS) Network, used magnetic resonance imaging (MRI) to demonstrate that the amygdala grows too rapidly in infancy. Overgrowth begins between six and 12 months of age, prior to the age when the hallmark behaviors of autism fully emerge, enabling the earliest diagnosis of this condition. Increased growth of the amygdala in infants who were later diagnosed with autism differed markedly from brain-growth patterns in babies with another neurodevelopmental disorder, fragile X syndrome, where no differences in amygdala growth were observed.
Published in the American Journal of Psychiatry, the official journal of the American Psychiatric Association, this research demonstrated that infants with fragile X syndrome already exhibit cognitive delays at six months of age, whereas infants who will later be diagnosed with autism do not show any deficits in cognitive ability at six months of age, but have a gradual decline in cognitive ability between six and 24 months of age, the age when they were diagnosed with Autism Spectrum Disorder in this study. Babies who go on to develop autism show no difference in the size of their amygdala at six months. However, their amygdala begins growing faster than other babies (including those with fragile X syndrome and those who do not develop autism), between six and 12 months of age, and is significantly enlarged by 12 months. This amygdala enlargement continues through 24 months, an age when behaviors are often sufficiently evident to warrant a diagnosis of autism.
Linking Amygdala Growth to Social Deficits in Autism
“We also found that the rate of amygdala overgrowth in the first year is linked to the child’s social deficits at age two,” said first author Mark Shen, PhD, Assistant Professor of Psychiatry and Neuroscience at UNC Chapel Hill and faculty of the Carolina Institute for Developmental Disabilities (CIDD). “The faster the amygdala grew in infancy, the more social difficulties the child showed when diagnosed with autism a year later.”
This research – the first to document amygdala overgrowth before symptoms of autism appear – was conducted through The Infant Brain Imaging Study (IBIS) Network, a consortium of 10 universities in the United States and Canada funded through a National Institutes of Health Autism Center of Excellence Network grant.
The researchers enrolled a total of 408 infants, including 58 infants at increased likelihood of developing autism (due to having an older sibling with autism) who were later diagnosed with autism, 212 infants at increased likelihood of autism but who did not develop autism, 109 typically developing controls, and 29 infants with fragile X syndrome. More than 1,000 MRI scans were obtained during natural sleep at six, 12, and 24 months of age.
So, what might be happening in the brains of these children to trigger this overgrowth and then the later development of autism? Scientists are starting to fit the pieces of that puzzle together.
Earlier studies by the IBIS team and others have revealed that while the social deficits that are a hallmark of autism are not present at six months of age, infants who go on to develop autism have problems as babies with how they attend to visual stimuli in their surroundings. The authors hypothesize that these early problems with processing visual and sensory information may place increased stress on the amygdala, leading to overgrowth of the amygdala.
Amygdala overgrowth has been linked to chronic stress in studies of other psychiatric conditions (e.g., depression and anxiety) and may provide a clue to understanding this observation in infants who later develop autism.
Early Autism Intervention
Senior author Joseph Piven, M.D., Professor of Psychiatry and Pediatrics at the University of North Carolina at Chapel Hill added, “Our research suggests an optimal time to start interventions and support children who are at highest likelihood of developing autism may be during the first year of life. The focus of a pre-symptomatic intervention might be to improve visual and other sensory processing in babies before social symptoms even appear.”
Reference: “Subcortical Brain Development in Autism and Fragile X Syndrome: Evidence for Dynamic, Age- and Disorder-Specific Trajectories in Infancy” by Mark D. Shen, Ph.D., Meghan R. Swanson, Ph.D., Jason J. Wolff, Ph.D., Jed T. Elison, Ph.D., Jessica B. Girault, Ph.D., Sun Hyung Kim, Ph.D., Rachel G. Smith, B.A., Michael M. Graves, M.S., Leigh Anne H. Weisenfeld, M.S.W., Lisa Flake, M.S.W., Leigh MacIntyre, M.S., Julia L. Gross, B.S., Catherine A. Burrows, Ph.D., Vladimir S. Fonov, Ph.D., D. Louis Collins, Ph.D., Alan C. Evans, Ph.D., Guido Gerig, Ph.D., Robert C. McKinstry, M.D., Ph.D., Juhi Pandey, Ph.D., Tanya St. John, Ph.D., Lonnie Zwaigenbaum, M.D., Annette M. Estes, Ph.D., Stephen R. Dager, M.D., Robert T. Schultz, Ph.D., Martin A. Styner, Ph.D., Kelly N. Botteron, M.D., Heather C. Hazlett, Ph.D. and Joseph Piven, M.D. for the IBIS Network, 25 March 2022, American Journal of Psychiatry.
DOI: 10.1176/appi.ajp.21090896
This research could not be possible without all the families and children who have participated in the IBIS study. Research sites included UNC-Chapel Hill, Washington University in St. Louis, Children’s Hospital of Philadelphia, McGill University, and University of Washington. This research was supported by grants from the Eunice Kennedy Shriver National Institute of Child Health and Human Development, National Institute of Environmental Health Sciences, and National Institute of Mental Health (R01-HD055741, R01-HD059854, R01-MH118362-01, R01-MH118362-02S1, T32-HD040127, U54-HD079124, K12-HD001441, R01-EB021391, U54-HD086984; NIH P50 HD103573), along with Autism Speaks and the Simons Foundation.
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.