
A lab-grown “mini spinal cord” just showed that futuristic “dancing molecules” might help heal paralysis.
Researchers at Northwestern University have created the most sophisticated lab grown model of human spinal cord injury so far.
In the new study, scientists worked with human spinal cord organoids grown from stem cells. These miniature, simplified versions of the spinal cord allowed the team to recreate different forms of spinal cord trauma and evaluate a promising regenerative treatment.
For the first time, the organoids closely reproduced the major features of spinal cord injury seen in people. That included widespread cell death, inflammation, and glial scarring. Glial scars are thick clusters of scar tissue that form after injury and create both physical and chemical barriers that block nerve repair.
When the damaged organoids were treated with “dancing molecules” — a therapy that previously reversed paralysis and repaired tissue in animal studies — the results were striking. The injured tissue produced significant neurite outgrowth, meaning the long extensions of neurons began growing again. Scar like tissue was greatly reduced. The findings strengthen hopes that the treatment, which recently received Orphan Drug Designation from the U.S. Food and Drug Administration (FDA), could improve recovery for people living with spinal cord injuries.
The study will be published today (February 11) in the journal Nature Biomedical Engineering.

“One of the most exciting aspects of organoids is that we can use them to test new therapies in human tissue,” said Northwestern’s Samuel I. Stupp, the study’s senior author and inventor of dancing molecules. “Short of a clinical trial, it’s the only way you can achieve this objective. We decided to develop two different injury models in a human spinal cord organoid and test our therapy to see if the results resembled what we previously saw in the animal model. After applying our therapy, the glial scar faded significantly to become barely detectable, and we saw neurites growing, resembling the axon regeneration we saw in animals. This is validation that our therapy has a good chance of working in humans.”
Stupp is a leader in self assembling materials and regenerative medicine. He serves as the Board of Trustees Professor of Materials Science and Engineering, Chemistry, Medicine and Biomedical Engineering at Northwestern, with appointments in the McCormick School of Engineering, Weinberg College of Arts and Sciences and Feinberg School of Medicine. He also directs the Center for Regenerative Nanomedicine (CRN). The study’s first author is Nozomu Takata, a research assistant professor of medicine at Feinberg and member of CRN.
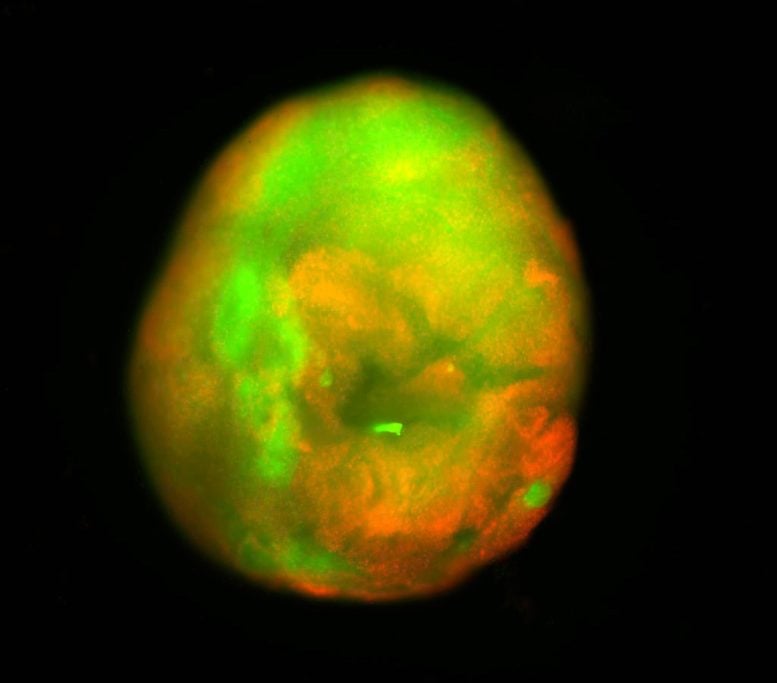
How Lab Grown Organoids Mimic Spinal Cord Injury
Organoids are created from induced pluripotent stem cells and grown in the laboratory. While they are not full organs, they replicate many key structural and functional features of real human tissue. Because they resemble actual organs at the cellular level, organoids are powerful tools for studying disease, exploring development, and testing potential treatments. They also offer a faster and less costly alternative to animal or human trials.
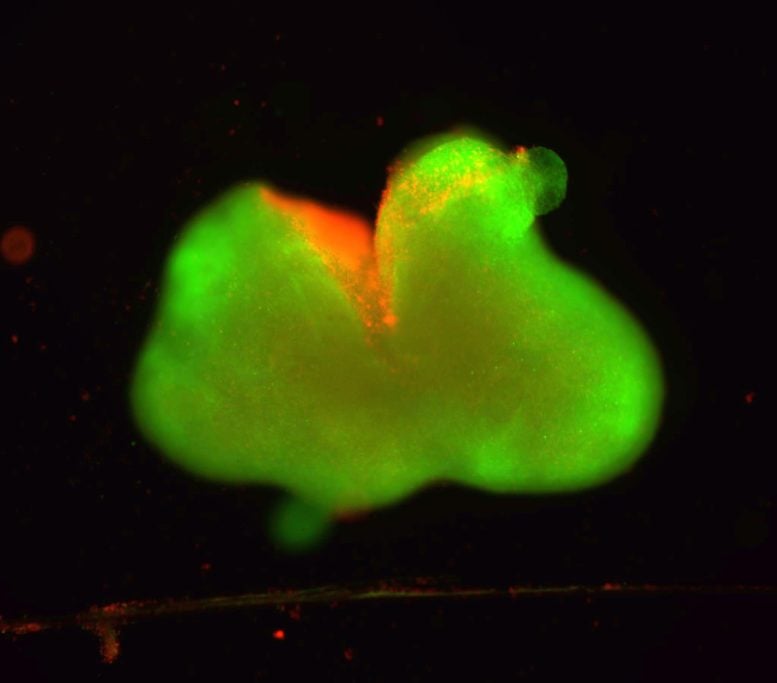
Although other teams have developed spinal cord organoids to study basic biology, this model marks a major advance for injury research. The organoids measured several millimeters across and were mature enough to withstand and model traumatic damage.
Over several months, the researchers carefully nurtured the stem cells so the organoids developed neurons and astrocytes, both essential cell types in the spinal cord. For the first time, the team also incorporated microglia — immune cells in the central nervous system — to better simulate the inflammatory response that follows spinal cord trauma.
“It’s kind of a pseudo-organ,” Stupp said. “We were the first to introduce microglia into a human spinal cord organoid, so that was a huge accomplishment. It means that our organoid has all the chemicals that the resident immune system produces in response to an injury. That makes it a more realistic, accurate model of spinal cord injury.”
What Are Dancing Molecules
After building a mature organoid, the team moved on to testing injuries and treatment. First introduced in 2021, the dancing molecules therapy is designed to harness molecular motion to repair tissue and potentially reverse paralysis after traumatic spinal cord injury. It is part of a broader platform known as supramolecular therapeutic peptides (STPs), which use large assemblies of 100,000 or more molecules to activate cell receptors and stimulate natural repair processes. (The concept of supramolecular therapies also is used in current GLP-1 drugs for weight loss and diabetes, an area that Stupp’s lab investigated nearly 15 years ago.)
The treatment is delivered as a liquid injection. Once inside the tissue, it quickly forms a network of nanofibers that resembles the spinal cord’s extracellular matrix. By adjusting how rapidly the molecules move within this network, the researchers improved how effectively the therapy interacts with constantly shifting cell receptors.
“Given that cells themselves and their receptors are in constant motion, you can imagine that molecules moving more rapidly would encounter these receptors more often,” Stupp said in 2021. “If the molecules are sluggish and not as ‘social,’ they may never come into contact with the cells.”
Earlier animal experiments showed that a single injection given 24 hours after a severe injury enabled mice to walk again within four weeks. Faster moving molecular formulations produced stronger therapeutic effects than slower ones, suggesting that increased motion improves cellular signaling and overall repair.
Testing the Regenerative Therapy on Injured Tissue
To simulate spinal cord trauma, the researchers created two common types of injury in the organoids. Some were carefully cut with a scalpel to mimic a laceration similar to a surgical wound. Others were subjected to compressive contusion injuries, resembling damage that might occur during a serious car crash or fall.
Both types of trauma triggered cell death and the formation of glial scars — hallmarks of real spinal cord injury.
“We could distinguish between the astrocytes that are a part of normal tissue and the astrocytes in the glial scar, which are large and very densely packed,” Stupp said. “We also detected the production of chondroitin sulfate proteoglycans, which are molecules in the nervous system that respond to injury and disease.”
When the dancing molecules therapy was applied to the injured organoids, it formed a supportive scaffold within the tissue. The treatment reduced inflammation, shrank glial scars, stimulated neurite extension, and encouraged neurons to grow in organized patterns.
Neurites include axons, which are often severed during spinal cord injuries. When axons are cut, communication between neurons is disrupted, leading to paralysis and loss of sensation below the injury site. Encouraging neurite regrowth could reconnect these neural pathways and potentially restore lost function.
The Role of Molecular Motion
Stupp believes the key to the therapy’s success lies in its supramolecular motion, or the ability of the molecules to move rapidly and even briefly detach from the nanofiber network. Experiments on healthy organoids reinforced that idea.
“Before we even developed the injury model, we tested the therapy on a healthy organoid,” he said. “The dancing molecules spun out all these long neurites on the surface of the organoid but, when we used molecules that had less or no motion, we saw nothing. This difference was very vivid.”
Looking ahead, the team plans to design even more advanced organoids to refine their injury models. They also aim to create versions that replicate long-standing chronic injuries, which typically involve thicker, more persistent scar tissue. In the future, these lab-grown spinal cords could even support personalized medicine by generating implantable tissue from a patient’s own stem cells, reducing the risk of immune rejection.
Reference: “Injury and therapy in a human spinal cord organoid” by Nozomu Takata, Zhiwei Li, Anna Metlushko, Feng Chen, Nicholas A. Sather, Xinyi Lin, Matthew J. Schipma, Oscar A. Carballo-Molina, Cassandre Jamroz, Madison E. Strong, Cara S. Smith, Yang Yang, Ching M. Wai, Neha Joshi, Jack Kolberg-Edelbrock, Kyle J. Gray, Suitu Wang, Liam C. Palmer and Samuel I. Stupp, 11 February 2026, Nature Biomedical Engineering.
DOI: 10.1038/s41551-025-01606-2
The study was supported by the Center for Regenerative Nanomedicine at Northwestern University and a gift from the John Potocsnak Family for spinal cord injury research.
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.
2 Comments
How do I volunteer to be tested on?
Great but already happened. A Brazilian Dr has made a quadriplegic walk again with polilaminina, a protein from human placenta. Her name is Dr Tatiana Lobo Coelho de Sampaio. Look her up at google: “dra tatiana coelho brazil” and you will discover that she cured a man half a year ago.