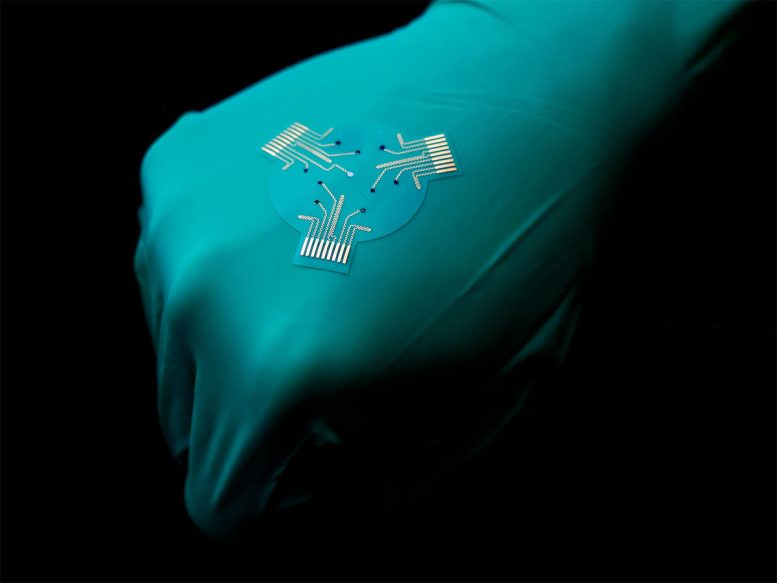
Smart Bandage Combines Monitoring, Medication, and Stimulation To Treat Chronic Wounds Efficiently
In general, the body’s natural healing process can effectively handle cuts, scrapes, burns, and other types of wounds. However, for individuals with diabetes, this may not always be the case. The condition can impair the healing process and result in persistent wounds that are susceptible to infection and may worsen over time.
Chronic wounds not only cause significant physical and emotional distress for those affected, but they also place a significant financial burden on healthcare systems. In the United States alone, the cost of treating these wounds amounts to an estimated $25 billion annually.
A new kind of smart bandage developed at Caltech may make treatment of these wounds easier, more effective, and less expensive. These smart bandages were developed in the lab of Wei Gao, assistant professor of medical engineering, Heritage Medical Research Institute Investigator, and Ronald and JoAnne Willens Scholar.
“There are many different types of chronic wounds, especially in diabetic ulcers and burns that last a long time and cause huge issues for the patient,” Gao says. “There is a demand for technology that can facilitate recovery.”
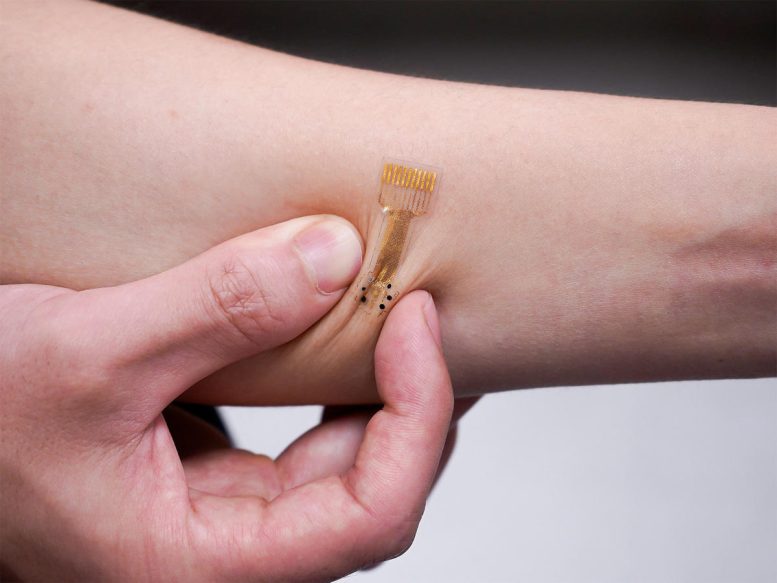
How the Smart Bandage Works
Unlike a typical bandage, which might only consist of layers of absorbent material, the smart bandages are made from a flexible and stretchy polymer containing embedded electronics and medication. The electronics allow the sensor to monitor for molecules like uric acid or lactate and conditions like pH level or temperature in the wound that may be indicative of inflammation or bacterial infection.
The bandage can respond in one of three ways: First, it can transmit the gathered data from the wound wirelessly to a nearby computer, tablet, or smartphone for review by the patient or a medical professional. Second, it can deliver an antibiotic or other medication stored within the bandage directly to the wound site to treat the inflammation and infection. Third, it can apply a low-level electrical field to the wound to stimulate tissue growth resulting in faster healing.
In animal models under laboratory conditions, the smart bandages showed the ability to provide real-time updates about wound conditions and the animals’ metabolic states to researchers, as well as offer speed healing of chronic infected wounds similar to those found in humans.

Gao says the results are promising and adds that future research in collaboration with the Keck School of Medicine of USC will focus on improving the bandage technology and testing it on human patients, whose therapeutic needs may be different than those of lab animals.
“We have shown this proof of concept in small animal models, but down the road, we would like to increase the stability of the device but also to test it on larger chronic wounds because the wound parameters and microenvironment may vary from site to site,” he says.
Reference: “A stretchable wireless wearable bioelectronic system for multiplexed monitoring and combination treatment of infected chronic wounds” by Ehsan Shirzaei Sani, Changhao Xu, Canran Wang, Yu Song, Jihong Min, Jiaobing Tu, Samuel A. Solomon, Jiahong Li, Jaminelli L. Banks, David G. Armstrong and Wei Gao, 24 March 2023, Science Advances.
DOI: 10.1126/sciadv.adf7388
The study was funded by the National Institutes of Health, the National Science Foundation, the Office of Naval Research, the Heritage Medical Research Institute, the Donna and Benjamin M. Rosen Bioengineering Center at Caltech, the Rothenberg Innovation Initiative at Caltech, and a Sloan Research Fellowship.
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.