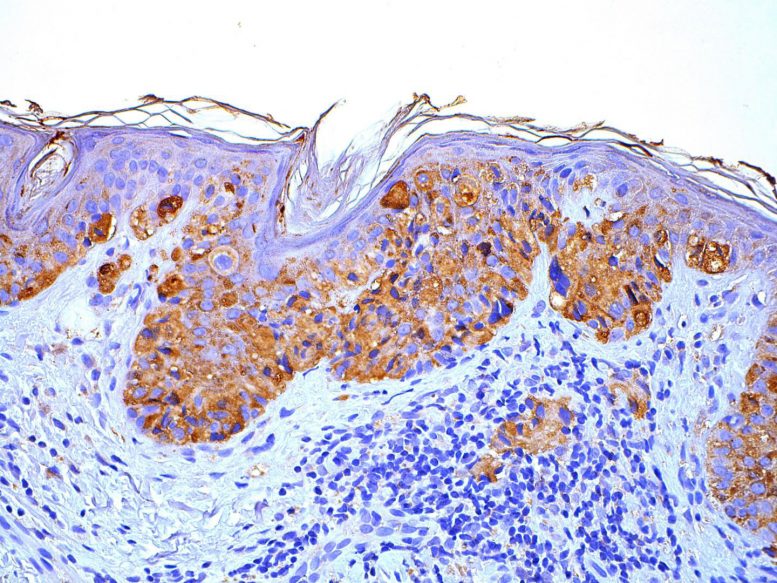
Researchers in the Perelman School of Medicine at the University of Pennsylvania have identified a new therapeutic target for the treatment of melanoma. For decades, research has associated female sex and a history of previous pregnancy with better outcomes after a melanoma diagnosis. Now, a research team from Perelman School of Medicine at the University of Pennsylvania says it may have determined the reason for the melanoma-protective effect. The mechanism is related to a cellular protein called the G protein-coupled estrogen receptor (GPER). When GPER was activated and combined with anti-PD-1 inhibitor drugs in mouse cancer models, the therapy dramatically extended survival in all animals and completely eliminated the tumor in 50 percent of the mice. Researchers published their findings in the journal eLife today.
Melanoma is the deadliest form of skin cancer, despite accounting for only about one percent of skin cancers overall. Rates of melanoma have been rising for 30 years, and the American Cancer Society estimates there were more than 87,000 new cases in the United States in 2017. Even with recent advances in immunotherapy, the majority of patients with metastatic forms of melanoma will die from their disease.
“In melanoma and many other types of cancer, women have a better prognosis than men, and women with a history of pregnancy seem to have a better prognosis than those women that have never been pregnant,” said the study’s senior author Todd W. Ridky, MD, Ph.D., an assistant professor of Dermatology at Penn. “Decades of research certainly suggests that there is something about female sex and pregnancy hormones that helps protect against melanoma, but no one really understood how that might work.”
Researchers say the key is GPER, a receptor found on melanocytes, which are pigment-producing cells in the skin. The receptor is normally activated by estrogen, which is higher in females, especially during pregnancy. Activation of GPER likely explains why many women notice that many areas of their skin get darker during pregnancy. Previous research from the Ridky lab has shown the effects of GPER activation are totally different than the effects of classical estrogen receptor signaling, which is important in breast cancer. The team discovered that melanocytes do not even express the classical estrogen receptor, and that all estrogen effects were the result of GPER.
In melanoma specifically, once GPER is activated, the cancer cell becomes more differentiated. This means it divides less frequently, makes more pigment, and becomes more visible and vulnerable to the natural immune system. This makes it harder for the cancer to become resistant to immunotherapies.
No drugs specifically target GPER, but Ridky and his team used a lab compound called G-1, originally developed by Eric Prossnitz, Ph.D., at the University of New Mexico Comprehensive Cancer Center, to stimulate GPER in mice, and then used anti-PD-1 inhibitors to treat the melanoma. The approach eliminated the tumors in half of all mice. The authors note that anti-PD-1 inhibitors, when used alone in mice with melanoma, extend survival modestly, but do not completely eliminate tumors, and no animals survive long-term.
“We hope this work inspires other researchers to revisit old ideas of differentiation-based cancer therapies now that immune therapies are available,” said the study’s lead author Christopher A. Natale, a researcher in Ridky’s lab. “It is clear that the future of cancer therapy lies in combination treatments, and differentiation drivers may be a very useful component in future cancer therapy regimens.”
As Ridky points out, this represents a unique approach to immunotherapy and cancer therapy in general.
“So much of the cancer field is focused on inhibitors, but in this new treatment approach, we’re actually activating something rather than blocking it,” Ridky said. “We used a synthetic compound to mimic part of what happens naturally during pregnancy, and as a result, the GPER activator is very well tolerated without any obvious toxic side effects that are common with most cancer drugs.”
Ridky also said this approach could be promising beyond melanoma.
“This is a receptor that is expressed in many organs, so there’s a reasonable expectation that this may work in other tumor types too,” Ridky said.
Although researchers did not observe any toxicities from the compound in mice, though they say they plan further toxicity studies before hopefully moving on to human trials.
Reference: “Activation of G protein-coupled estrogen receptor signaling inhibits melanoma and improves response to immune checkpoint blockade” by Christopher A Natale, Jinyang Li, Junqian Zhang, Ankit Dahal, Tzvete Dentchev, Ben Z Stanger and Todd W Ridky, 16 January 2018, eLife.
DOI: 10.7554/eLife.31770
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.