Breast cancer in younger women is more common—and more aggressive—than current screening guidelines suggest. Stable trends across 11 years show a need for earlier, personalized risk evaluation.
A review of data from seven outpatient centers in the New York region shows that 20 to 24% of all breast cancers detected over an 11-year period occurred in women between ages 18 and 49. These findings are being presented today at the annual meeting of the Radiological Society of North America (RSNA).
“This research shows that a significant proportion of cancers are diagnosed in women under 40, a group for whom there are no screening guidelines at this time,” said Stamatia Destounis, M.D., radiologist Elizabeth Wende Breast Care (EWBC) in Rochester, New York. “Consideration must be given by physicians caring for women in this age group to performing risk assessment in order to identify those who may benefit from more intensive screening due to being higher risk.”
National data has been pointing toward a gradual increase in breast cancer among younger women, which has led experts to rethink age-based screening recommendations and how risk levels are determined.
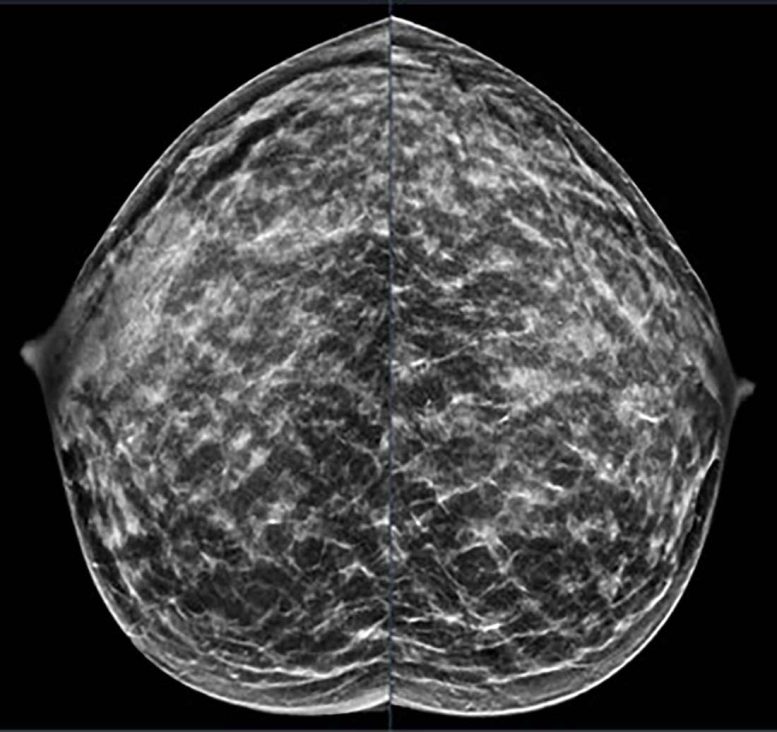
Current Screening Guidelines and Gaps for Younger Patients
For women considered average risk, the U.S. Preventive Services Task Force recommends mammography every other year beginning at age 40 and continuing through age 74. The American Cancer Society advises annual mammograms starting at age 45, with the option to begin between ages 40 to 44. Women with higher risk due to specific factors may be advised to undergo both breast MRI and mammography each year starting at about age 30, but no official screening guidelines currently exist for women younger than that.
Study Methods and Data Collection
Dr. Destounis and EWBC research manager Andrea L. Arieno, B.S., set out to identify breast cancer cases diagnosed from 2014 through 2024 across seven outpatient facilities covering a 200-mile area in Western New York. All cancers in patients aged 18 to 49 were reviewed using clinical imaging reports.
“We specifically collected details on how the cancer was found (screening or diagnostic), the type of cancer, and other tumor characteristics,” Dr. Destounis said. “We excluded cases that were not primary breast cancer. We analyzed trends over time by age subgroups, detection method, and tumor biology. This helped us to identify how breast cancer presents in this patient population, how frequently it occurs, and the types of tumors found.”
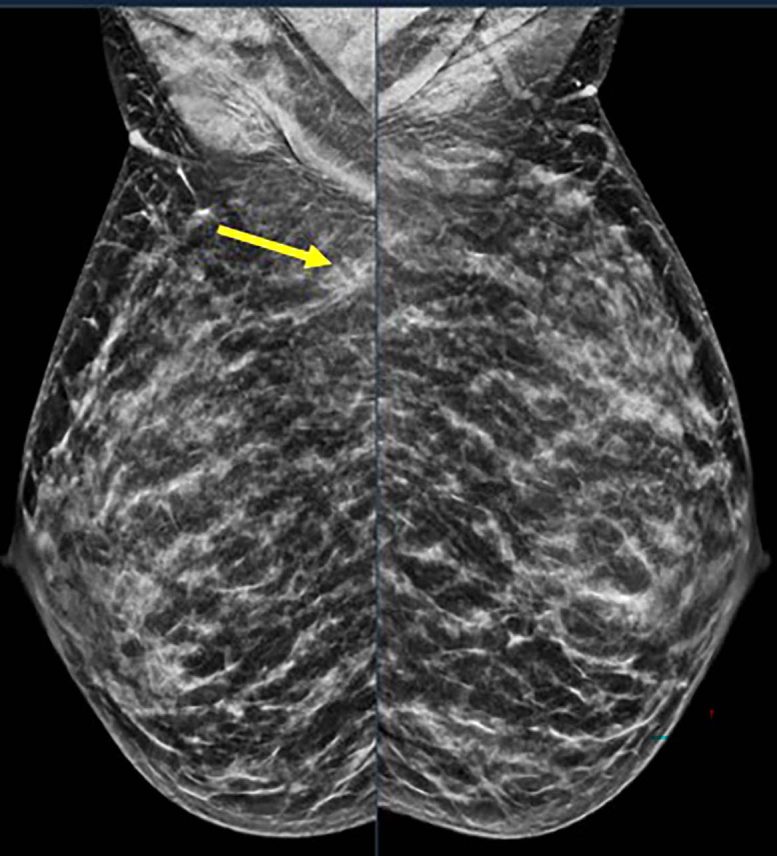
Most Tumors Were Invasive and Often Aggressive
The researchers documented 1,799 breast cancers in 1,290 women aged 18 to 49. Annual diagnoses in this group ranged from 145 to 196. The average age at diagnosis was 42.6 years (range 23 to 49). Of these cancers, 731 (41%) were identified during screening and 1,068 (59%) through diagnostic evaluation. A total of 1,451 cases (80.7%) were invasive, while 347 (19.3%) were non-invasive.
“Most of these cancers were invasive, meaning they could spread beyond the breast, and many were aggressive types—especially in women under 40,” Dr. Destounis said. “Some were ‘triple-negative,’ a form of breast cancer that is harder to treat because it doesn’t respond to common hormone-based therapies.”
Younger Women Represent a Consistent Share of Diagnoses
Although women younger than 50 made up only 21% to 25% of screened patients each year, they consistently accounted for about one quarter of all breast cancers detected.
“This is striking because it shows that younger women not only carry a stable and substantial share of the breast cancer burden, but their tumors are often biologically aggressive,” she said. “That combination—steady incidence plus disproportionately aggressive biology—directly challenges age-based screening cutoffs and strengthens the case for earlier, risk-tailored screening approaches.”
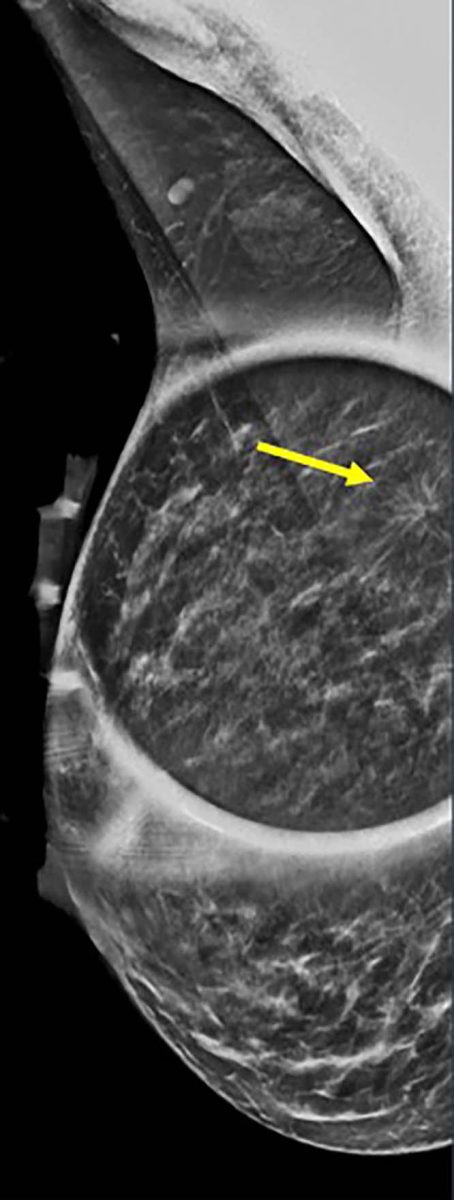
Stable Numbers Suggest a Persistent Long-Term Issue
According to Dr. Destounis, one of the most important observations from the study is that the number of breast cancers in younger women stayed stable throughout the research period. Even though fewer young women may have been seen at certain times, the total number of cancers in this group did not decline.
“That means this problem is not going away,” she said. “It is here to stay and needs to be addressed on a larger scale. Research such as this supports earlier and tailored screening to allow for earlier detection and better treatment outcomes. This data reinforces that women under 50, especially those under 40, shouldn’t be seen as ‘low risk’ by default and can absolutely benefit from risk assessment being performed as early as possible.”
Higher-Risk Groups and Early Awareness
Dr. Destounis advised that younger individuals should understand the importance of being aware of breast changes and starting screening in certain situations.
“Those with a strong family history or genetic mutation, as well as certain minorities and ethnic backgrounds, are at higher risk for breast cancer at a younger age,” she said.
Age Alone Cannot Determine Screening Needs
Dr. Destounis emphasized that the study’s key message is that breast cancer in younger women is not uncommon and, when present, is often more serious.
“We can’t rely only on age alone to decide who should be screened,” she said. “Paying closer attention to personal and family history, and possibly screening earlier for some women, could help detect these cancers sooner.”
Meeting: 111th Scientific Assembly and Annual Meeting of the Radiological Society of North America (RSNA)
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.
2 Comments
Carcinogenic (cancer-causing) chemicals.
What percent of those got the jab?