
Harmful proteins are also produced by glial cells.
Memory loss, confusion, and speech difficulties are hallmark symptoms of Alzheimer’s disease, the leading cause of dementia, which currently affects around 35 million people globally, with numbers on the rise. Central to the disease is the naturally occurring brain protein, amyloid beta, which accumulates into insoluble clumps in affected individuals. These clumps form plaques between neurons, leading to neuronal damage.
Researchers at the Max Planck Institute (MPI) for Multidisciplinary Sciences have now shown that, in addition to neurons, special glial cells in the brain also produce amyloid beta. This finding could open up new avenues for future therapies.
There is no cure for Alzheimer’s disease. However, there are therapeutic approaches to reduce the amyloid plaques in the brain. That can slow down the progression of the disease, but it cannot reverse or stop it.
“Until now, neurons were thought to be the main producers of amyloid beta and have been the main target for new drugs,” explains Klaus-Armin Nave, Director at the MPI for Multidisciplinary Sciences. Results from his Department of Neurogenetics have now shown: In addition to neurons, special glial cells – called oligodendrocytes – play an important role in plaque formation.
“One of the tasks of oligodendrocytes is to form myelin – an insulating layer – and wrap it around the nerve fibers to speed up signal transmission,” explains Andrew Octavian Sasmita, one of the first authors of the study now published in Nature Neuroscience and a former PhD student in Nave’s team. In a previous study, the Göttingen researchers had already discovered that defective myelin of oligodendrocytes exacerbates Alzheimer’s disease. Do glial cells play an even greater role in the disease than previously thought?
“We have now shown that although neurons are the main producers of amyloid beta, oligodendrocytes also produce a significant amount of the protein which is incorporated into plaques,” says Sasmita. A research group led by Marc Aurel Busche of the University College London (England) recently came to similar conclusions.
Preventing plaque formation
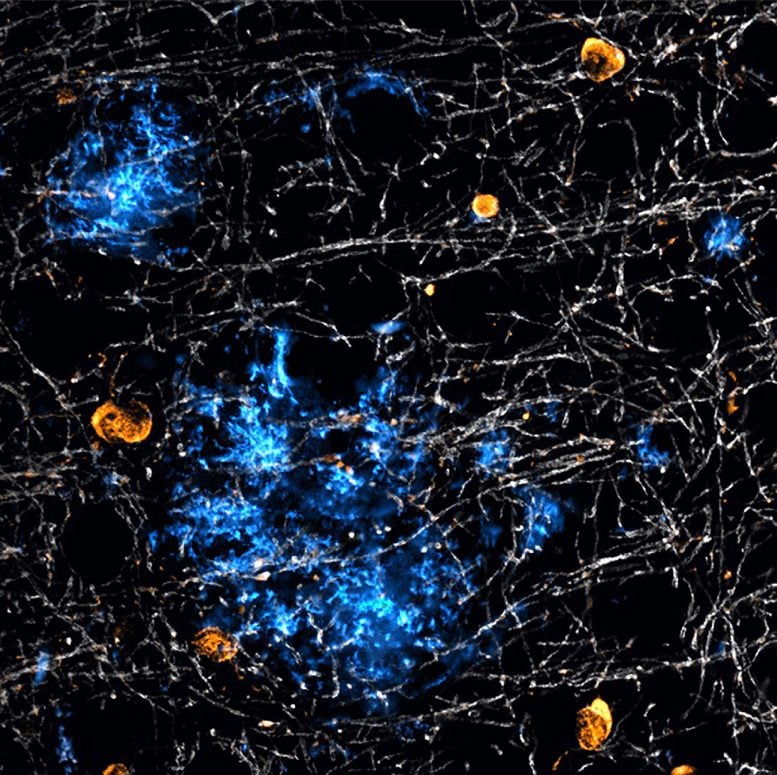
The cells of the nervous system produce amyloid beta by cleaving a larger precursor molecule with the help of an enzyme called BACE1. For their experiments, the researchers specifically knocked out BACE1 in the neurons and oligodendrocytes of mice. They then used 3D light-sheet microscopy to study plaque formation throughout the brain, providing a complete picture of amyloid plaques in all brain regions.
“Oligodendrocytes lacking BACE1 developed about 30 percent fewer plaques. Knocking out the BACE1 gene in neurons reduced plaque formation by over 95 percent,” says Constanze Depp, also a first author of the study and a former PhD student in Nave’s department. The scientists also found out: “Plaque deposits only form when a certain amount of neuronal amyloid beta is present. The oligodendrocytes then contribute to these plaques.”
This threshold could be useful for Alzheimer’s therapies. “If we can successfully inhibit BACE1 before this threshold is reached, the plaques might form later,” Nave emphasizes. That could help to slow down the progression of Alzheimer’s disease at an early stage.
Reference: “Oligodendrocytes produce amyloid-β and contribute to plaque formation alongside neurons in Alzheimer’s disease model mice” by Andrew Octavian Sasmita, Constanze Depp, Taisiia Nazarenko, Ting Sun, Sophie B. Siems, Erinne Cherisse Ong, Yakum B. Nkeh, Carolin Böhler, Xuan Yu, Bastian Bues, Lisa Evangelista, Shuying Mao, Barbara Morgado, Zoe Wu, Torben Ruhwedel, Swati Subramanian, Friederike Börensen, Katharina Overhoff, Lena Spieth, Stefan A. Berghoff, Katherine Rose Sadleir, Robert Vassar, Simone Eggert, Sandra Goebbels, Takashi Saito, Takaomi Saido, Gesine Saher, Wiebke Möbius, Gonçalo Castelo-Branco, Hans-Wolfgang Klafki, Oliver Wirths, Jens Wiltfang, Sarah Jäkel, Riqiang Yan and Klaus-Armin Nave, 5 August 2024, Nature Neuroscience.
DOI: 10.1038/s41593-024-01730-3
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.
3 Comments
I am a medical anthropologist researcher studying the cultural causes of disease. The authors admit that they don’t know the cause of Alzheimer’s, and are focusing on the biochemistry of rodent brains. They should focus on the biomechanics of how humans sleep and the effect of gravity on brain circulation. Sleep position is a critical issue for brain health, and we have done research showing that the way you sleep can cause a host of brain problems associated with high intracranial pressure and low brain circulation, which can be the cause of plaque formation and dementia, as well as causing migraines, glaucoma, sleep apnea, stroke, ADHD, and more. Slightly elevating the head of the bed, as you would with a wedge for acid reflux, increases brain circulation and has an almost immediate impact within days. It also helps with reducing sinus congestion in the morning, reduces puffy eyes, and makes you more alert. NASA scientists know this from zero gravity research, since astronauts experience fluid shifting to the head with zero gravity, causing a host of brain, ear, and eye problems. They study this effect by having people on Earth lie flat. They discovered 30 degree head of bed elevation is optimal for brain and heart circulation, but trying 10 degrees of elevation will make a huge difference after one night!
See my article, Heads Up! The Way You Are Sleeping May Be Killing You. https://www.academia.edu/1483361/Heads_Up_The_Way_You_Are_Sleeping_May_Be_Killing_You_
Thank you Sydney for an informative and sensible comment. I have elevated my head for many years to avoid GERD and aspiration and I am glad to know it has some added benefits.
That ridiculous AI illustration that leads this article does NOT reflect Alzheimer’s at all. That guy just learned his wife is divorcing him thus giving him a blinding migraine headache.