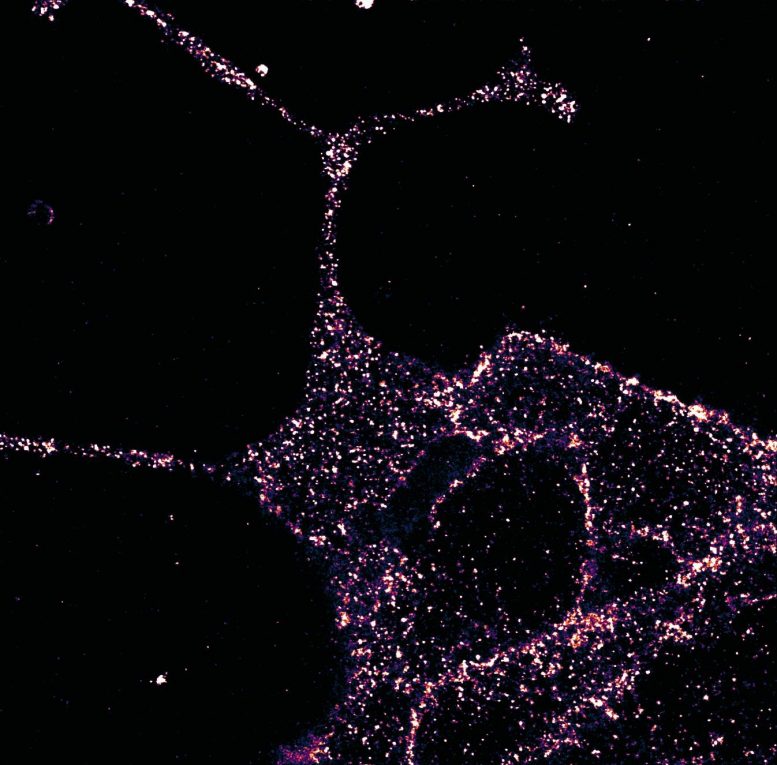
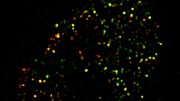
GLP1R visualized in insulin-secreting beta cells at super-resolution. Credit: University of Birmingham
Scientists have examined a key receptor for the first time at high resolution — broadening understanding of how it might function, and opening the door to future improvements in treating conditions such as type 2 diabetes.
Glucagon-like peptide-1 receptors (GLP1R) are found on insulin-producing beta cells of the pancreas and neurons in the brain. The receptor encourages the pancreas to release more insulin, stops the liver from producing too much glucose, and reduces appetite. This combination of effects can help to control blood sugar levels.
As such, GLP1R has become a significant target for the treatment of type 2 diabetes, and a range of drugs are now available that are based on it. But much remains unknown about GLP1R function because its small size makes it difficult to visualize.
An international group of scientists led by experts at the University of Birmingham and the Max Planck Institute for Medical Research, Heidelberg, have now conducted a detailed examination of the receptor in living cells.
Researchers used a number of techniques — including synthesis of marker compounds, immunostaining, super-resolution microscopy, as well as ‘in vivo’ examination of mice. They were able to label GLP1R with their developed fluorescent probes so as to show its location in the cells and its response to signal molecules.
Publishing their findings in Nature Communications, the researchers — who were partly funded by Diabetes UK — note that they now provide a comprehensively tested and unique GLP1R detection toolbox, which has updated our view of this receptor, with implications for the treatment of conditions such as obesity and type 2 diabetes.
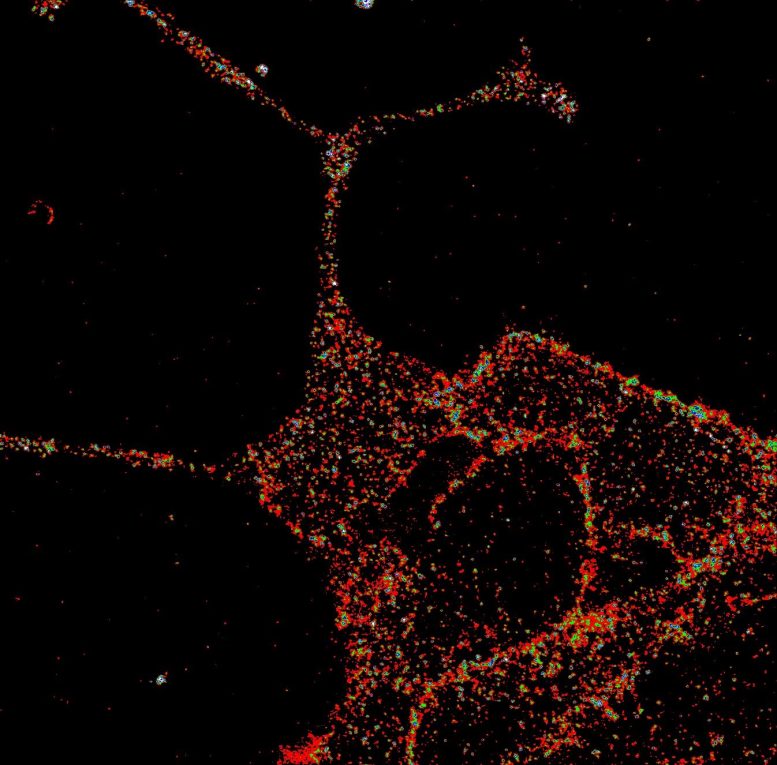
GLP1R visualized in insulin-secreting beta cells at super-resolution. Credit: University of Birmingham
David Hodson, Professor of Cellular Metabolism, at the University of Birmingham, commented: “Our research allows us to visualize this key receptor in much more detail than before. Think about watching a movie in standard definition versus 4k, that’s how big the difference is. We believe this breakthrough will give us a much greater understanding of GLP1R distribution and function. Whilst this will not immediately change treatment for patients, it might influence how we design drugs in the future.”
Johannes Broichhagen, Departmental Group Leader of the Max-Planck Institute for Medical Research, commented: “Our experiments, made possible by combining expertise in chemistry and cell biology, will improve our understanding of GLP1R in the pancreas and the brain. Our new tools have been used in stem cells and in the living animal to visualize this important receptor, and we provide the first super-resolution characterization of a class B GPCR. Importantly, our results suggest a degree of complexity not readily appreciated with previous approaches.”
Dr. Elizabeth Robertson, Director of Research at Diabetes UK commented: “The effects of type 2 diabetes are serious and widespread, so finding more effective treatments to help people manage their condition and reduce their risk of its potentially devastating complications is absolutely vital.
“Through innovative research like this, we can get to grips with key aspects of type 2 diabetes in unprecedented detail, and blaze a trail towards better treatments.”
GLP1R is a member of the so-called G protein-coupled receptors (GPCRs), which play a role in many of the body’s functions. An increased understanding of how they work has greatly affected modern medicine, and today, it is estimated that between one-third and one-half of all marketed drugs act by binding to GPCRs.
Reference: “Super-resolution microscopy compatible fluorescent probes reveal endogenous glucagon-like peptide-1 receptor distribution and dynamics” by Julia Ast, Anastasia Arvaniti, Nicholas H.F. Fine, Daniela Nasteska, Fiona B. Ashford, Zania Stamataki, Zsombor Koszegi, Andrea Bacon, Ben J. Jones, Maria A. Lucey, Shugo Sasaki, Daniel I. Brierley, Benoit Hastoy, Alejandra Tomas, Giuseppe D’Agostino, Frank Reimann, Francis C. Lynn, Christopher A. Reissaus, Amelia K. Linnemann, Elisa D’Este, Davide Calebiro, Stefan Trapp, Kai Johnsson, Tom Podewin, Johannes Broichhagen and David J. Hodson, 24 January 2020, Nature Communications.
DOI: 10.1038/s41467-020-14309-w
The research was funded by Diabetes UK, Medical Research Council (MRC) and European Research Council (ERC).





Be the first to comment on "High-Definition View of Diabetes-Related Proteins Obtained, Opening the Door to Future Treatments"