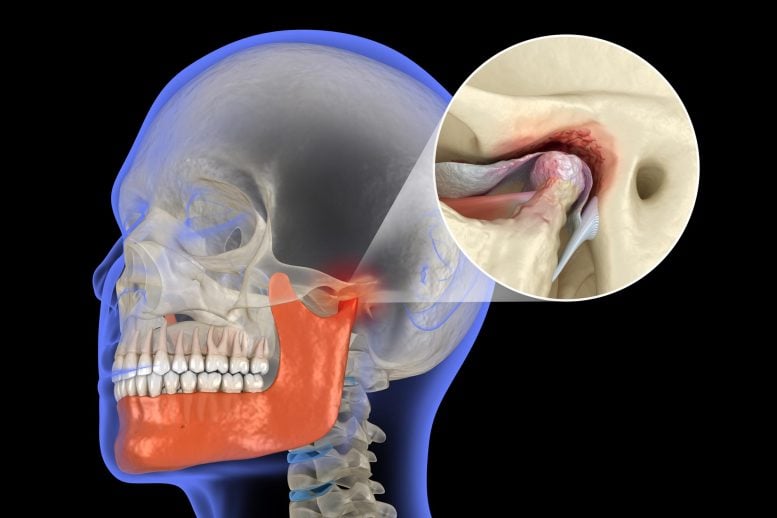
A newly identified molecular player may help explain how cartilage in the jaw joint resists inflammatory damage.
Every time you chew, speak, or yawn, your jaw depends on a small but hardworking joint that has to move smoothly under constant pressure. That motion is possible because cartilage and a disc inside the joint help absorb force and reduce friction. When that protective tissue starts to break down, the result can be stiffness, inflammation, and serious pain.
This is what happens in temporomandibular joint osteoarthritis (TMJ-OA), a degenerative condition that damages the cartilage of the temporomandibular joint (TMJ), the hinge-like joint that connects the lower jaw to the skull. It is a frustrating condition not only because it can interfere with everyday life, but also because cartilage has a limited ability to repair itself once damaged.
Despite how common TMJ-OA is, there are currently no FDA-approved medications designed specifically to protect or rebuild cartilage in this joint. Researchers at Boston University have now identified a promising biological factor that may help address this gap. Their study shows that an enzyme called lysyl oxidase-like 2 (LOXL2) plays an important role in preserving cartilage and preventing arthritis-like damage.
Investigating the Role of LOXL2
The research was led by Assistant Professor Manish V. Bais with collaborators from Boston University and the University of Pittsburgh, USA. Their findings were published online in the International Journal of Oral Science.
To examine how LOXL2 affects cartilage, the scientists used genetically modified mice that lacked the Loxl2 gene. They also analyzed cartilage samples taken from goats, whose jaw joints share many structural similarities with human jaw joints. This combination of models allowed the team to study how the enzyme influences cartilage health and degeneration.
“Cartilage deterioration is a hallmark of osteoarthritis,” notes Prof. Bais. Normally, the cartilage tissue is maintained by a group of specialized cells called chondrocytes. But during osteoarthritis, this balance is disrupted, and inflammatory molecules, like interleukin-1 beta (IL-1β), start activating destructive pathways inside the joint.
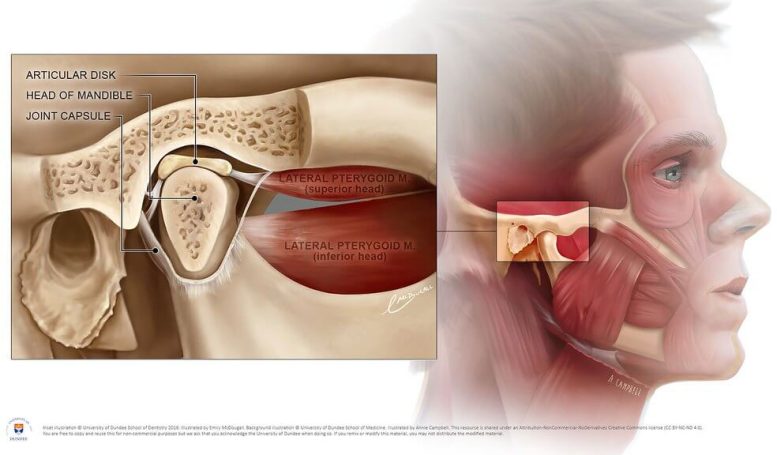
“We observed that the loss of loxl2 activates inflammatory genes and weakens the cartilage by reducing its essential structural components such as aggrecanproteoglycans and promote inflammatory factors,” explains Prof. Bais
To determine how this damage occurs, the researchers examined the NF-κB (nuclear factor kappa B) signaling pathway. This pathway is often described as a “master switch” that controls inflammation in many tissues. Once activated, it directs cells to produce substances that intensify tissue injury.
The team discovered that LOXL2 helps keep this pathway under control. By suppressing NF-κB activity, the enzyme reduces inflammation and prevents chondrocytes from dying. It also protects mitochondria, the structures inside cells that generate energy, from inflammatory damage while maintaining their activity and energy production. As a result, cartilage cells remain functional even when exposed to inflammatory stress.
Potential Pathway Toward New Treatments
When researchers treated cartilage samples with extra LOXL2, the enzyme reversed several damaging effects caused by inflammation. Levels of molecules linked to pain and cartilage breakdown, including MMP13, ADAMTS5, and PTGS2, dropped significantly. At the same time, protective components of the cartilage tissue were restored.
Similar results were observed in goat cartilage samples, strengthening the potential clinical relevance of the findings. Goat temporomandibular joints are structurally comparable to human jaw joints, which makes them useful for studying TMJ disorders.
“Our findings identify LOXL2 as a promising therapeutic target for TMJ disorders. By safeguarding cartilage and preventing cell death, this enzyme may have the potential to slow down or even stop the progression of arthritis in the jaw,” emphasizes Prof. Bais.
The researchers note that further clinical studies will be necessary to confirm whether the same effects occur in people. Even so, the findings represent an important step toward therapies designed specifically for TMJ disorders. Such treatments could help preserve joint function, reduce pain, and improve quality of life for patients affected by jaw arthritis.
Reference: “LOXL2 deletion triggers TMJ osteoarthritis, while overexpression protects it from NF-κB-induced chondrocyte apoptosis” by Rajnikant Dilip Raut, Chumki Choudhury, Faiza Ali, Amit kumar Chakraborty, Mohammed Moeeduddin Ahmed, Cheyleann Del Valle Ponce De Leon, Harshal V. Modh, Pushkar Mehra, Yuwei Fan, Alejandro Almarza and Manish V. Bais, 4 February 2026, International Journal of Oral Science.
DOI: 10.1038/s41368-025-00409-0
The study was funded by the National Institutes of Health.
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.
1 Comment
Sunny Tennyson