Research shows NSAIDs like ibuprofen and naproxen fail to reduce inflammation or slow knee osteoarthritis progression.
Taking anti-inflammatory pain relievers like ibuprofen and naproxen for osteoarthritis may worsen inflammation in the knee joint over time. This is according to a new scientific study being presented at the annual meeting of the Radiological Society of North America (RSNA) next week.
As the most common form of arthritis, osteoarthritis (OA) affects more than 32 million adults in the U.S. and more than 500 million people worldwide. It occurs most frequently in the hands, hips, and knees. In people with osteoarthritis, the cartilage that cushions the joint gradually wears away. This is why it is sometimes called degenerative joint disease or “wear and tear” arthritis. Arthritis is often accompanied by inflammation, or swelling, of the joint, which can be painful.
Non-steroidal anti-inflammatory drugs (NSAIDs) are commonly prescribed for osteoarthritis pain and inflammation. Common NSAIDs include Ibuprofen (Advil, Motrin) and naproxen (Aleve). However, little is known about the long-term effects of these drugs on disease progression.
“To date, no curative therapy has been approved to cure or reduce the progression of knee osteoarthritis,” said the study’s lead author, Johanna Luitjens, postdoctoral scholar in the Department of Radiology and Biomedical Imaging at the University of California, San Francisco. “NSAIDs are frequently used to treat pain, but it is still an open discussion of how NSAID use influences outcomes for osteoarthritis patients. In particular, the impact of NSAIDs on synovitis, or the inflammation of the membrane lining the joint, has never been analyzed using MRI-based structural biomarkers.”
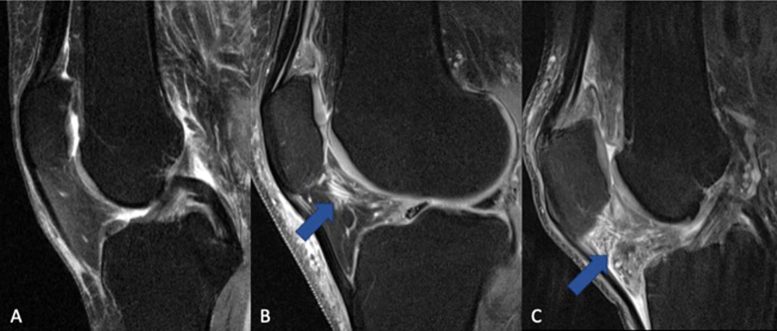
Dr. Luitjens and colleagues set out to analyze the association between NSAID use and synovitis in patients with osteoarthritis of the knee and to assess how treatment with NSAIDs affects joint structure over time.
“Synovitis mediates development and progression of osteoarthritis and may be a therapeutic target,” Dr. Luitjens said. “Therefore, the goal of our study was to analyze whether NSAID treatment influences the development or progression of synovitis and to investigate whether cartilage imaging biomarkers, which reflect changes in osteoarthritis, are impacted by NSAID treatment.”
No Protective Benefit from NSAIDs
For the study, 277 participants from the Osteoarthritis Initiative cohort with moderate to severe osteoarthritis and sustained NSAID treatment for at least one year between baseline and four-year follow-up were included in the study and compared with a group of 793 control participants who were not treated with NSAIDs. All participants underwent 3T MRI of the knee initially and after four years. Images were scored for biomarkers of inflammation.
Cartilage thickness, composition, and other MRI measurements served as noninvasive biomarkers for evaluating arthritis progression.
The results showed no long-term benefit of NSAID use. Joint inflammation and cartilage quality were worse at baseline in the participants taking NSAIDs, compared to the control group, and worsened at four-year follow-up.
“In this large group of participants, we were able to show that there were no protective mechanisms from NSAIDs in reducing inflammation or slowing down the progression of osteoarthritis of the knee joint,” Dr. Luitjens said. “The use of NSAIDs for their anti-inflammatory function has been frequently propagated in patients with osteoarthritis in recent years and should be revisited, since a positive impact on joint inflammation could not be demonstrated.”
According to Dr. Luitjens, there are several possible reasons why NSAID use increases synovitis.
“On the one hand, the anti-inflammatory effect that normally comes from NSAIDs may not effectively prevent synovitis, with progressive degenerative change resulting in worsening of synovitis over time,” she said. “On the other hand, patients who have synovitis and are taking pain-relieving medications may be physically more active due to pain relief, which could potentially lead to worsening of synovitis, although we adjusted for physical activity in our model.”
Dr. Luitjens noted that prospective, randomized studies should be performed in the future to provide conclusive evidence of the anti-inflammatory impact of NSAIDs.
Co-authors are Charles McCulloch, Ph.D., Thomas Link, M.D., Ph.D., Felix Gassert, M.D., Gabby Joseph, Ph.D., and John Lynch, Ph.D.
Meeting: 108th Scientific Assembly and Annual Meeting of the Radiological Society of North America
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.
17 Comments
Taking 500mg of Tylenol with 800 mg of motrin once a day; together is the only combination of medication that gives me relief. Opiates don’thelp.
Is it harmful long term to take tylenol with motrin once a day for arthritic pain?
Taking ibuprofen for pain resulted in my chronic kidney disease, according to a nephrologist.
I’m an RN with arthritis. I want to work, but pain keeps me from it. I spoke to my MD about my excruciating pain on multiple visits. He chose to no longer be my MD.
I cannot find anything OTC to help me.
Almost died due to intestinal bleeding from taking ibuprofen for knee pain relief. Do NOT take daily, it can kill you!!!
To me it is cause and effect. I’ve used a heating pad for over 30 years that often put my joints in remission. Unfortunately, it is a painful process but if I persevere the pain goes away. Behaves like a virus.
Lately, because I’m old, 84, my muscles have started to shrink. This loads up the joint and restricts motion. I found heating the muscles, seems to relax them, relieving the joint pressure. Exercise is the best medicine.
A combination of naturopathic and physio approaches seems better. Physio approach is to build muscle around the joints to reduce the stress on the joint from moderate activity. Naturopathic diet to include anti inflammatory ingredients like ginger and tumeric (and other vegetables and herbs).
A combination of naturopathic and physio approaches seems better. Physio approach is to build muscle around the joints to reduce the stress on the joint from moderate activity. Naturopathic diet to include anti inflammatory ingredients like ginger and tumeric (and other vegetables and herbs).
I’m a 83 year old tennis player who has played tournaments from the age of 12 and still play a couple of national doubles tournaments a year. In my late 30’s I began taking Ibuprofen for generalized stiffness after matches which progressed to not playing a tournament without taking my Ibuprofen. I felt like it was a miracle drug and not only was there less pain but my flexibility definitely increased. (I was world senior 55 champion). I have had pretty bad osteoarthritis since my 50’s and cannot function without daily NSAID’s. In fact several years ago when preparing for a surgical procedure I had to stop my Ibuprofen and by the 5th day I was paralyzed and couldn’t get off the couch! This scared the hell out of me! I called the doctor and asked if I could take acetaminophen and he concurred. Within a couple of hours I was able to get off the couch and even went to dinner with my daughter,however wobbly. I was so scared after that incident that I never want to be without an NSAID again!!
After researching them more, I’ve switched to Naproxen because I feel it has less chance of a cardiovascular event.
Read up on PRP platlet rich plasma.its a life saver.
CBD topical cream or gel works great!
I take Alleve twice a day for 3-5 days and go off it for 2 weeks before I resume taking it (for lower back pain)
pain)m
the big word here is MAY….
The only thing that helps my knee and lower back pain is strength training legs, back and core. My GI told me that taking anti-inflammatory pain killers will destroy your stomach lining. He can see damage after 3 days’ use.
I body slammed on my back slipping on Ice a week ago Friday! Saturday morning I had to Call the Ambulance! I’ve been on a Fusion List since 2019 so was not impressed and did some serious pleadings with God before getting up from the snow and ice. Tylenol was offered @ the Hospital but I didn’t engage as at 70 I don’t even have anything like that in my Home. My daughter had some Advil delivered Sunday, but a couple day’s later when coming down from it’s relief the spasms seemed to worsen so I decided to STOP it’s use! In August 2003 I was in a Cluster of Tradesmen exposed to Pulp Mill Emissions and 500 TPD of ToXic Methanol was Listed in the Emissions by Environment Canada! Tylenol is derived from Toxic Methanol and my throat mouth and tongue were burning my last day of work! A year later in September I got Gassed again @ another Pulp Mill and Vehicle Exhaust started onsetting the same sequalae of symptoms as the year before, burning throat mouth and tongue and Cardiac stress! I was dying Driving to work so started going to the Library instead!
The Chemical Chain for Toxic Methanol is Formaldehyde which metabolizes to Formic acid in the Liver > LACTIC ACID in ALL our Cells! Formic acid is what was causing the burning throat! My cellular Lactic acid spiked so high I suffered MELAS after eating a Yougurt! Two nights before I had burning throat etc after eating Honey on Toast and Research lead to the Pesticide Division of Environment Canada allowing Bee Keeper’s to use Formic acid in their Hives to K’ the Varoa Mite! Toxic Methanol is what is used to make Bio-diesel from Restaurant Grease! And E85 Ethanol entrained Gasoline emits 50% more Formaldehyde than Conventional Gasoline! So Environmentally and in our Phood we are increasingly elevating our Cellular Lactic acid levels, to the point I was suffering Lactic acidosis a level of Kidney disease! I started volunteering at an Injured Worker’s Support Group and observed Worker’s with multiple injuries Prescribed acetaminophen based opiods progress into Chronic Fatigue and then Fibromyalgia! With the metabolism of Formic acid biochemically converting to Lactic acid it wasn’t difficult to join the dots on muscle burn!
Many of my customers are using a 30mg Full Spectrum CBD softgel to avoid NSAIDs. One customer in particular came off of 15 Tylenol per day to just 2 of the softgels.
AuntBonnies.com
I’ve never this stuff work yet. Maybe if you have a good imagination?