New findings reveal that untreated obstructive sleep apnea can significantly raise the likelihood of developing Parkinson’s disease, but consistent CPAP use appears to dramatically cut that risk.
Scientists suspect that repeated nightly drops in oxygen put long-term strain on neurons, potentially contributing to neurodegeneration. The results highlight how something as simple as improving sleep quality may offer powerful protection against conditions once thought largely inevitable with age.
Sleep Apnea Linked to Higher Parkinson’s Risk
New findings indicate that individuals who leave obstructive sleep apnea untreated face a greater likelihood of developing Parkinson’s disease. Improving sleep quality through the use of continuous positive airway pressure, or CPAP, can meaningfully lower this risk.
The work, published today (November 24) in JAMA Neurology, analyzed electronic health records from more than 11 million U.S. military veterans who received care through the Department of Veterans Affairs between 1999 and 2022.
Scientists from Oregon Health & Science University and the Portland VA Health Care System led the investigation.
Parkinson’s is a progressive neurological disorder that affects roughly 1 million people in the United States, and the odds of developing it gradually increase with age, particularly after 60.
Age-Related Rise in Parkinson’s Cases
The new research points to a long-term elevation in Parkinson’s risk among people whose sleep apnea goes untreated.
After accounting for factors such as obesity, age, and high blood pressure, investigators still identified a clear association between untreated sleep apnea and Parkinson’s. In this large population of veterans with sleep apnea, those who did not use CPAP had nearly twice the likelihood of developing Parkinson’s compared with individuals who used the therapy.
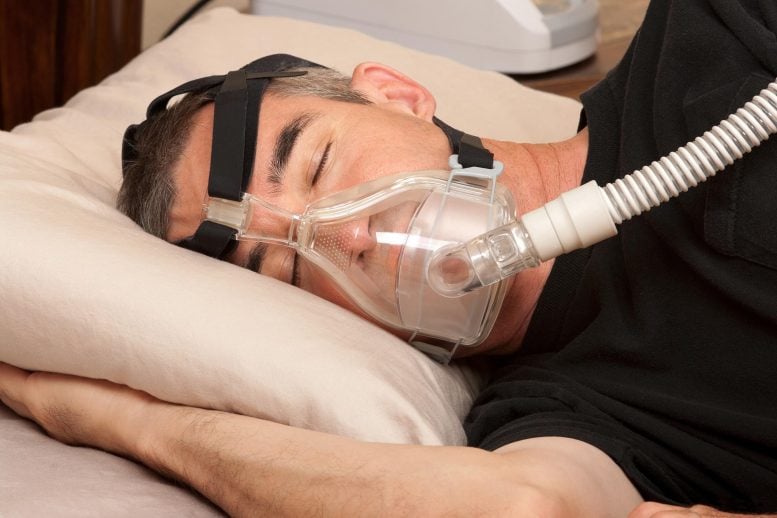
Untreated Apnea Nearly Doubles Parkinson’s Odds
“It’s not at all a guarantee that you’re going to get Parkinson’s, but it significantly increases the chances,” said co-author Gregory Scott, M.D., Ph.D., assistant professor of pathology in the OHSU School of Medicine and a pathologist at the VA Portland.
Sleep apnea occurs when a person’s breathing repeatedly pauses and resumes during the night, which can limit the amount of oxygen the body receives.
How Oxygen Deprivation May Harm Neurons
“If you stop breathing and oxygen is not at a normal level, your neurons are probably not functioning at a normal level either,” said lead author Lee Neilson, M.D., assistant professor of neurology at OHSU and a staff neurologist at the Portland VA. “Add that up night after night, year after year, and it may explain why fixing the problem by using CPAP may build in some resilience against neurodegenerative conditions, including Parkinson’s.”
Sleep Quality as a Neuroprotective Tool
Neilson said he intends to prioritize the health benefits of sound sleep with his patients, especially in view of the research revealing an elevated risk of Parkinson’s.
“I think it will change my practice,” he said.
Scott noted that even though some people with sleep apnea resist treatment with CPAP, he pointed to the experience of many veterans who swear by it.
Veterans’ Positive Experiences with CPAP
“The veterans who use their CPAP love it,” he said. “They’re telling other people about it. They feel better, they’re less tired. Perhaps if others know about this reduction in risk of Parkinson’s disease, it will further convince people with sleep apnea to give CPAP a try.”
Reference: “Obstructive Sleep Apnea, Positive Airway Pressure, and Implications of Early Treatment in Parkinson Disease” by Lee E. Neilson, Isabella Montaño, Jasmine L. May, Savanah Sicard, Yeilim Cho, Jeffrey J. Iliff, Jonathan E. Elliott, Miranda M. Lim and Gregory D. Scott, 24 November 2025, JAMA Neurology.
DOI: 10.1001/jamaneurol.2025.4691
In addition to Scott and Neilson, co-authors include Isabella Montano, B.A., Jasmin May, M.D., Ph.D., Jonathan Elliott, Ph.D., and Miranda Lim, M.D., Ph.D., of OHSU and the Portland VA Health Care System; and Yeilim Cho, M.D., and Jeffrey Iliff, Ph.D., of the University of Washington and the VA Puget Sound Health Care System.
The research was supported by the VA, grant awards BX005760, CX00253, I01RX004822, I01RX005371, CX002022, BX006155 and Bx006155; the John and Tami Marick Family Foundation, the Collins Medical Trust; the National Institute on Aging of the National Institutes of Health, award P30AG066518; and the U.S. Army Medical Research Acquisition Activity, 820 Chandler Street, Fort Detrick, Maryland 21702-5014, under award numbers HT9425-24-1-0774 and HT9425-24-1-0775. Opinions, interpretations, conclusions and recommendations are those of the authors and are not necessarily endorsed by the Department of Defense, the NIH, VA or other funders.
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.
2 Comments
Great Article filled with very informative awareness.
Just sleep on your side.