Researchers have found that focusing powerful non-invasive magnet stimulation on a specific brain area can improve the symptoms of Obsessive Compulsive Disorder (OCD). This opens the way to treat the large minority of sufferers who do not respond to conventional treatment. The work is presented at the ECNP Conference in Copenhagen*.
OCD is broadly defined as recurrent thoughts or urges, or excessive repetitive behaviors which an individual feels driven to perform. Around 12 adults in every thousand suffer from OCD in any given year, although 2.3% of adults will suffer at some point in their life. It is generally treated through exposure and response prevention (ERP) therapy (which exposes the patient to the content of his obsessions\urges without performing the compulsions) and medication, such as SSRIs (Selective Serotonin Reuptake Inhibitors e.g. fluoxetine (Prozac/Sarafem) or Sertraline (Paxil) or Serotonin Reuptake Inhibitors e.g. clomipramine (Anafranil), however between a third and a half of patients don’t respond well to treatment
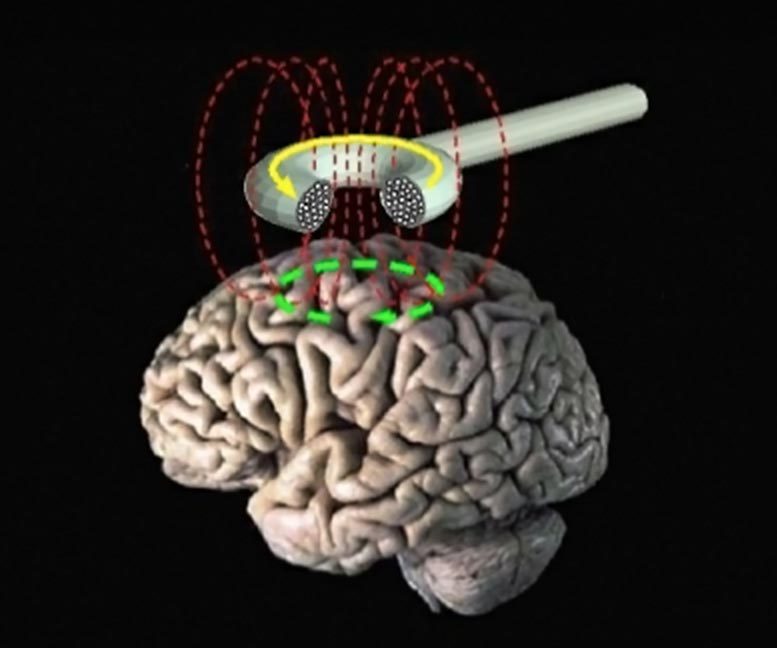
Deep Transcranial Magnetic Stimulation (dTMS) is a type of brain stimulation technique where pulsed magnetic fields are generated by a coil placed on the scalp. This field activates the neuronal circuits at the target brain area, resulting in symptom improvement. It is clinically used for the treatment of some difficult cases of depression.
Dr. Lior Carmi (along with Prof. Joseph Zohar and Prof. Abraham Zangen), from the Chaim Sheba Medical Center in Israel, led an international group of scientists in a multi-center randomized controlled trial (RCT) spread over 11 centers. 99 patients with Obsessive Compulsive Disorder were assigned to either be treated with dTMS, or to receive pretend treatment (sham treatment). All the patients in the trial had previously failed to respond to antidepressant treatment.
Dr. Carmi said “An interesting point about this trial is that we deliberately provoked the patients for about 5 minutes before each dTMS session. We did this by tailoring a provocation for each patient according to their own specific OCD obsessions. For example, if someone had obsessions about getting contaminated, we exposed him to a situation in which these obsessions were aroused, for instance, touching a bathroom door handle or the trash can. Another example would be if someone had obsessions regarding not closing the water tap at home, we deliberately aroused the doubt about that. All these exposures were designed for each individual patient. During the first meeting with the patient, we learned his symptoms and created a list of which exposures to use during the study. The idea is to deliver the treatment when the brain circuitry is aroused and not while the patient is thinking about the shopping he needs to do after the session will be over”.
The sessions consisted of 6 weeks of daily dTMS (20Hz) treatment focused on specific areas of the brain related to OCD**. This is the first time these areas have been targeted for this disorder. The degree of response was measured using the generally-accepted Yale-Brown Obsessive Compulsive Scale (YBOCS) questionnaire. After 6 weeks, 38% of those being treated responded to the treatment. They showed an average reduction of more than 30% in symptom severity, as opposed to 11% of patients receiving the sham treatment.
A month after treatment finished the response rate was 45.2% in the active group versus 17.8% in the sham group. Around a third of both the treated group and the untreated group complained of headaches, but only 2 dropped out over the trial due to pain.
Lior Carmi said, “Researchers have tested TMS for OCD in the past, but this is the first time we have stimulated this region of the brain and done so while we tailored exposures to each patient. In addition, we have done so using a standardized protocol in a multi-center randomized trial (at 11 cities in the U.S, Canada and Israel). This means that we have achieved these positive results although the variety of patients and variety of clinicians who rated the response. Where the existing treatment works for OCD, it can work well; our method is primarily aimed at those who do not respond to conventional treatment”.
Commenting, Professor Jose M Menchon (Bellvitge University Hospital, University of Barcelona, Barcelona, Spain) said:
“This is a very exciting study because it shows positive results in OCD using deep transcranial magnetic stimulation. Until now, the clinical trials with TMS in OCD had been carried out with non-deep TMS, which may have limitations in its effect because the magnetic field can only reach the cortical surface. However, deep TMS allows reaching and modulating deeper brain regions that can be more critically involved in OCD. Deep TMS may become a useful therapeutic strategy if these positive results are confirmed in further studies”.
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.
5 Comments
Be interesting to try this on drug addicts
Now that’s a good idea. Have there been other studies that compare addiction to compulsive behavior? Is the same part of the brain involved?
That’s good to know. My name is Shey and I suffer with OCD,since the age of 16, but it has worsened in my now late fourties.
This could be the answer to a lot of people who don’t benifit from ssri treatment. My son was diagnosed at age 15. Finding help is like looking for a needle in a haystack.
The therapist my grandson has been seeing for one year is doing brain wave therapy…he also takes Zoloft that is approved for OCD…the therapy has reduced his symptoms over 75%..I also purchased the FisherWallace set to use at home