Note: There is now a newer Novel Coronavirus (COVID-19) Situation Report 83.
WHO Novel Coronavirus (COVID-19) Situation Report 82
- Yemen reported its first case of COVID-19 in the past 24 hours.
- WHO has developed the following definition for reporting COVID deaths: a COVID-19 death is defined for surveillance purposes as a death resulting from a clinically compatible illness in a probable or confirmed COVID-19 case, unless there is a clear alternative cause of death that cannot be related to COVID disease (e.g., trauma). There should be no period of complete recovery between the illness and death.
- WHO Director-General Dr. Tedros, in a press conference held yesterday, highlighted the issue of planning the transition out of stay-at-home restrictions: “WHO wants to see restrictions lifted as much as anyone. At the same time, lifting restrictions too quickly could lead to a deadly resurgence.” For more information, please see here.
- WHO has updated its Q&A page on COVID-19 to provide information of how the virus spreads and how it is affecting people worldwide. For more details, please see here.
- To date, there are a limited number of publications and national situation reports that provide information on the number of healthcare worker(HCW)infections. Understanding infection in HCWs is critical to informing the specific infection prevention and control measures needed to protect HCWs from infection. For more details, please see ‘Subject in Focus’ below.
Risk Assessment
Global Level: Very High
Coronavirus Situation in Numbers
Globally
- 1,610,909 confirmed cases (89,657) new)
- 99,690 deaths (6,892 new)
European Region
- 839,257 confirmed cases (39,561 new)
- 70,565 deaths (4,352 new)
Regions of the Americas
- 536,664 confirmed cases (43,491 new)
- 19,294 deaths (2,256 new)
Western Pacific Region
- 118,549 confirmed cases (1,302 new)
- 4,017 deaths (39 new)
Eastern Mediterranean Region
- 92,226 confirmed cases (3,569 new)
- 4,771 deaths (164 new)
South-East Asia
- 14,161 confirmed cases (1,183 new)
- 617 deaths (48 new)
African Region
- 9,340 confirmed cases (551 new)
- 415 deaths (33 new)
Subject in Focus: Infection in health care workers
Healthcare workers (HCWs) play an essential role at the front lines, providing care for patients. In the context of COVID-19 and during routine health services, they provide critical care to patients and ensure that infection prevention and control (IPC) measures are implemented and adhered to in healthcare facilities in order to limit healthcare-associated infections.
As of April 8, 2020, 22073 cases of COVID-19 among HCWs from 52 countries had been reported to WHO. However, at the present time, there is no systematic reporting of HCW COVID-19 infections to WHO and therefore this number probably under-represents the true number of COVID-19 HCW infections globally.
To date, there are a limited number of publications and national situation reports that provide information on the number of HCW infections. For example, a publication from China CDC on 44672 confirmed cases as of February 17, 2020, indicated 1,688 (3.8%) infections were among HCWs, including five deaths.1 In Italy, a situation report from April 10, 2020, reported 15,314 infections among HCW, representing 11% of all infections at that time.2 Further publications have described the epidemiological and clinical characteristics of infections among HCWs.3-7 While many infections are indicated as mild, severe outcomes, including deaths, among HCWs have also been reported.
Understanding infection in HCWs is critical to informing the specific IPC measures needed to protect HCWs from infection. A limited number of publications have identified risk factors for infection among HCWs. Preliminary results suggest HCWs are being infected both in the workplace and in the community, most often through infected family members.8 In healthcare settings, factors associated with HCW infection have included: late recognition or suspicion of COVID-19 in patients, working in a higher-risk department, longer duty hours, sub-optimal adherence to IPC measures such as hand hygiene practices, and lack of or improper use of personal protective equipment (PPE).9-10 Other factors have also been documented, such as inadequate or insufficient IPC training for respiratory pathogens, including the COVID-19 virus, as well as long exposure in areas in healthcare facilities where large numbers of COVID-19 patients were being cared for.
To prevent infection in healthcare settings, WHO recommends the use of contact and droplet precautions by HCWs caring for patients with COVID-19.11 WHO also recommends that airborne precautions be applied in settings in which procedures and support treatments that generate aerosols are performed.11 In this context, the correct use of PPE is critical, in particular wearing appropriate PPE for the clinical setting, paying special attention to procedures to put on and remove PPE correctly, and adhering to hand hygiene and other IPC measures. When these precautions are applied correctly and consistently, alongside standard precautions and administrative, engineering, and environmental controls, the risk for HCW infections is substantially reduced or avoided altogether.
WHO has also developed a risk assessment tool for exposed HCWs in a healthcare facility12 and a sero-epidemiological protocol to determine risk factors for infection among HCW13, and is finalizing an in-depth epidemiological surveillance tool for HCW infections. A number of countries are currently using these tools and protocols, and this information will be essential to understand the extent of infection among HCWs, the extent of transmission within healthcare facilities and the best approaches to protect HCWs against infection.
Finally, as HCWs caring for patients with COVID-19 are subject to long working hours, fatigue, occupational burn-out, stigma, physical and psychological violence, and back injury from patient handling, it is important that efforts be made to maintain the physical and mental health of HCWs and the quality of care. Therefore, WHO recommends that IPC measures be complemented by occupational safety and health measures, psycho-social support, adequate staffing levels, and clinical rotation, to reduce the risk of burn-out, for safe and healthy working environments and to respect the rights of health workers to decent working conditions.1
References
- The Novel Coronavirus Pneumonia Emergency Response Epidemiology Team. The epidemiological characteristics of an outbreak of 2019 Novel Coronavirus Diseases (COVID-19) –China, 2020. http://weekly.chinacdc.cn/en/article/id/e53946e2-c6c4-41e9-9a9b-fea8db1a8f51
- Integrated surveillance of COVID-19 in Italy: 10 April 2020. https://www.epicentro.iss.it/en/coronavirus/bollettino/Infografica_10aprile%20ENG.pdf
- Kluytmans M, Buiting A, Pas S, et al. SARS-CoV-2 infection in 86 healthcare workers in two Dutch hospitals in March 2020. medRxiv. 2020:2020.03.23.20041913. DOI: 10.1101/2020.03.23.20041913.
- Liu M, He P, Liu HG, et al. [Clinical characteristics of 30 medical workers infected with new coronavirus pneumonia]. Zhonghua Jie He He Hu Xi Za Zhi. 2020 Mar 12;43(3):209-14. DOI: 10.3760/cma.j.issn.1001-0939.2020.03.014. PMID: 32164090.
- Liu J, Ouyang L, Guo P, et al. Epidemiological, Clinical Characteristics and Outcome of Medical Staff Infected with COVID-19 in Wuhan, China: A Retrospective Case Series Analysis. medRxiv. 2020:2020.03.09.20033118. DOI: 10.1101/2020.03.09.20033118.
- McMichael TM, Currie DW, Clark S, et al. Epidemiology of Covid-19 in a Long-Term Care Facility in King County, Washington. New England Journal of Medicine. 2020 DOI: 10.1056/NEJMoa2005412.
- Wang C, Liu L, Hao X, et al. Evolving Epidemiology and Impact of Non-pharmaceutical Interventions on the Outbreak of Coronavirus Disease 2019 in Wuhan, China. medRxiv. 2020:2020.03.03.20030593. DOI: 10.1101/2020.03.03.20030593.
- World Health Organization. Report of the WHO-China Joint Mission on Coronavirus Disease 2019 (COVID-19) 16-24 February 2020 [Internet]. Geneva: World Health Organization; 2020 https://www.who.int/docs/default-source/coronaviruse/who-china-joint-mission-on-covid-19-final-report.pdf
- Ran L, Chen X, Wang Y, et al. Risk Factors of Healthcare Workers with Corona Virus Disease 2019: ARetrospective Cohort Study in a Designated Hospital of Wuhan in China. Clin Infect Dis. 2020 Mar 17 DOI: 10.1093/cid/ciaa287. PMID: 32179890.
- Lai J, Ma S, Wang Y, et al. Factors Associated WithMental Health Outcomes Among Health Care Workers Exposed to Coronavirus Disease 2019. JAMA Netw Open. 2020 Mar 2;3(3):e203976. DOI: 10.1001/jamanetworkopen.2020.3976. PMID: 32202646.
- World Health Organization. Infection prevention and control during health care when COVID-19 is suspected. https://www.who.int/publications-detail/infection-prevention-and-control-during-health-care-when-novel-coronavirus-(ncov)-infection-is-suspected-20200125
- World Health Organization. Risk assessment and management of exposure of health care workers in the context of COVID-19. https://apps.who.int/iris/bitstream/handle/10665/331496/WHO-2019-nCov-HCW_risk_assessment-2020.2-eng.pdf
- World Health Organization. Protocol for assessment of potential risk factors for 2019-novel coronavirus (2019-nCoV) infection among health care workers in a health care setting. https://www.who.int/publications-detail/protocol-for-assessment-of-potential-risk-factors-for-2019-novel-coronavirus-(2019-ncov)-infection-among-health-care-workers-in-a-health-care-setting
- World Health Organization. Coronavirus disease (COVID-19) outbreak: rights, roles and responsibilities of health workers, including key considerations for occupational safety and health, World Health Organization, Interim guidance 19 March 2020 https://www.who.int/publications-detail/coronavirus-disease-(covid-19)-outbreak-rights-roles-and-responsibilities-of-health-workers-including-key-considerations-for-occupational-safety-and-health
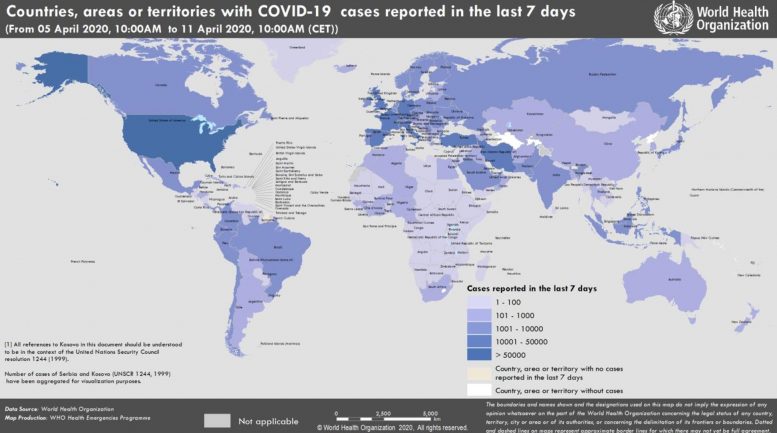
Countries, territories or areas with reported laboratory-confirmed COVID-19 cases and deaths, April 11, 2020
| Country/Territory/Area | Confirmed Cases |
|---|---|
| United States of America | 461275 |
| Spain | 157022 |
| Italy | 147577 |
| Germany | 117658 |
| France | 89683 |
| China | 83369 |
| United Kingdom | 70276 |
| Iran | 68192 |
| Turkey | 47029 |
| Belgium | 26667 |
| Switzerland | 24228 |
| Netherlands | 23097 |
| Canada | 21226 |
| Brazil | 17857 |
| Portugal | 15472 |
| Russian Federation | 13584 |
| Austria | 13560 |
| Republic of Korea | 10480 |
| Israel | 10095 |
| Sweden | 9685 |
| Ireland | 8089 |
| India | 7447 |
| Ecuador | 7161 |
| Chile | 6501 |
| Norway | 6244 |
| Australia | 6238 |
| Japan | 6005 |
| Poland | 5955 |
| Denmark | 5819 |
| Czechia | 5732 |
| Romania | 5467 |
| Peru | 5256 |
| Pakistan | 4788 |
| Malaysia | 4346 |
| Philippines | 4195 |
| Saudi Arabia | 3651 |
| Indonesia | 3512 |
| Mexico | 3441 |
| United Arab Emirates | 3360 |
| Luxembourg | 3223 |
| Serbia | 3105 |
| Finland | 2769 |
| Panama | 2752 |
| Thailand | 2518 |
| Qatar | 2512 |
| Ukraine | 2511 |
| Dominican Republic | 2349 |
| Colombia | 2223 |
| Singapore | 2108 |
| Greece | 2011 |
| South Africa | 2003 |
| Belarus | 1981 |
| Argentina | 1929 |
| Egypt | 1794 |
| Algeria | 1761 |
| Iceland | 1675 |
| Croatia | 1495 |
| Morocco | 1448 |
| Republic of Moldova | 1438 |
| Hungary | 1310 |
| Iraq | 1280 |
| Estonia | 1258 |
| Slovenia | 1160 |
| New Zealand | 1035 |
| Lithuania | 999 |
| Bahrain | 998 |
| Kuwait | 993 |
| Azerbaijan | 991 |
| Armenia | 937 |
| Bosnia and Herzegovina | 901 |
| Kazakhstan | 859 |
| Cameroon | 803 |
| Puerto Rico | 725 |
| Slovakia | 715 |
| International (Diamond Princess Cruise Ship) | 712 |
| North Macedonia | 711 |
| Tunisia | 671 |
| Bulgaria | 635 |
| Uzbekistan | 624 |
| Latvia | 612 |
| Lebanon | 609 |
| Andorra | 602 |
| Cyprus | 595 |
| Cuba | 564 |
| Oman | 546 |
| Costa Rica | 539 |
| Afghanistan | 521 |
| Côte d’Ivoire | 480 |
| Uruguay | 473 |
| Burkina Faso | 443 |
| Niger | 438 |
| Bangladesh | 424 |
| Albania | 416 |
| Honduras | 382 |
| Réunion | 382 |
| Ghana | 378 |
| Jordan | 372 |
| Malta | 350 |
| San Marino | 344 |
| Kyrgyzstan | 339 |
| Mauritius | 318 |
| Nigeria | 305 |
| Bolivia | 268 |
| Palestinian Territory | 268 |
| Senegal | 265 |
| Vietnam | 257 |
| Montenegro | 255 |
| Kosovo | 250 |
| Georgia | 233 |
| Democratic Republic of the Congo | 215 |
| Sri Lanka | 197 |
| Guinea | 194 |
| Guernsey | 191 |
| Mayotte | 191 |
| Isle of Man | 190 |
| Kenya | 189 |
| Faroe Islands | 184 |
| Jersey | 183 |
| Venezuela | 171 |
| Martinique | 154 |
| Djibouti | 150 |
| Guadeloupe | 143 |
| Brunei Darussalam | 136 |
| Guam | 130 |
| Paraguay | 129 |
| Guatemala | 126 |
| Cambodia | 120 |
| Rwanda | 118 |
| El Salvador | 117 |
| Gibraltar | 113 |
| Trinidad and Tobago | 109 |
| Madagascar | 95 |
| Aruba | 86 |
| French Guiana | 84 |
| Liechtenstein | 80 |
| Mali | 74 |
| Togo | 73 |
| Barbados | 66 |
| Ethiopia | 65 |
| Jamaica | 63 |
| Congo | 60 |
| Monaco | 54 |
| Uganda | 53 |
| French Polynesia | 51 |
| Sint Maarten | 50 |
| United States Virgin Islands | 50 |
| Bermuda | 48 |
| Cayman Islands | 45 |
| Gabon | 44 |
| Bahamas | 41 |
| Zambia | 40 |
| Guyana | 37 |
| Liberia | 37 |
| Guinea-Bissau | 35 |
| Eritrea | 33 |
| Saint Martin | 32 |
| United Republic of Tanzania | 32 |
| Benin | 30 |
| Haiti | 30 |
| Myanmar | 28 |
| Libya | 24 |
| Mozambique | 20 |
| Angola | 19 |
| Antigua and Barbuda | 19 |
| Maldives | 19 |
| Syrian Arab Republic | 19 |
| New Caledonia | 18 |
| Sudan | 17 |
| Dominica | 16 |
| Equatorial Guinea | 16 |
| Fiji | 16 |
| Lao People’s Democratic Republic | 16 |
| Mongolia | 16 |
| Namibia | 16 |
| Curaçao | 14 |
| Saint Lucia | 14 |
| Botswana | 13 |
| Eswatini | 12 |
| Grenada | 12 |
| Saint Vincent and the Grenadines | 12 |
| Somalia | 12 |
| Central African Republic | 11 |
| Chad | 11 |
| Greenland | 11 |
| Northern Mariana Islands | 11 |
| Saint Kitts and Nevis | 11 |
| Seychelles | 11 |
| Zimbabwe | 11 |
| Belize | 10 |
| Suriname | 10 |
| Malawi | 9 |
| Montserrat | 9 |
| Nepal | 9 |
| Holy See | 8 |
| Turks and Caicos | 8 |
| Cabo Verde | 7 |
| Mauritania | 7 |
| Nicaragua | 7 |
| Sierra Leone | 7 |
| Saint Barthelemy | 6 |
| Bhutan | 5 |
| Falkland Islands (Malvinas) | 5 |
| Gambia | 4 |
| São Tomé and Príncipe | 4 |
| Anguilla | 3 |
| British Virgin Islands | 3 |
| Burundi | 3 |
| South Sudan | 3 |
| Bonaire, Sint Eustatius and Saba | 2 |
| Papua New Guinea | 2 |
| Timor-Leste | 2 |
| Saint Pierre and Miquelon | 1 |
| Yemen | 1 |
| Total | 1610909 |
Recommendations and Advice for the Public
If you are not in an area where COVID-19 is spreading or have not traveled from an area where COVID-19 is spreading or have not been in contact with an infected patient, your risk of infection is low. It is understandable that you may feel anxious about the outbreak. Get the facts from reliable sources to help you accurately determine your risks so that you can take reasonable precautions (see Frequently Asked Questions). Seek guidance from WHO, your healthcare provider, your national public health authority or your employer for accurate information on COVID-19 and whether COVID-19 is circulating where you live. It is important to be informed of the situation and take appropriate measures to protect yourself and your family (see Protection measures for everyone).
If you are in an area where there are cases of COVID-19 you need to take the risk of infection seriously. Follow the advice of WHO and guidance issued by national and local health authorities. For most people, COVID-19 infection will cause mild illness however, it can make some people very ill and, in some people, it can be fatal. Older people, and those with pre-existing medical conditions (such as cardiovascular disease, chronic respiratory disease or diabetes) are at risk for severe disease (See Protection measures for persons who are in or have recently visited (past 14 days) areas where COVID-19 is spreading).
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.
1 Comment
Oh, how things have changed. Now there are over 500 million cases and 6 million deaths. I think it’s odd how in April 2020, everybody seemed more panicked about COVID. I wasn’t too worried about it because the likelihood of catching it was so low at the time. Now, a large portion of the worlds population has or has had it before and many died and people seem to think it’s no big deal. COVID fatigue I guess.