Researchers at Kyoto University have found that neutrophils, a type of white blood cell, can induce anti-inflammatory macrophages (M2) within granulomas, which are dense globular structures that form during chronic inflammation. This M2 macrophage polarization can help regulate inflammation and tissue health. The team believes that their findings, derived from studying tuberculosis, could also be applied to tumor development. By understanding how a bacteria-permissive microenvironment is formed, the researchers hope to contribute to more effective cancer drug development.
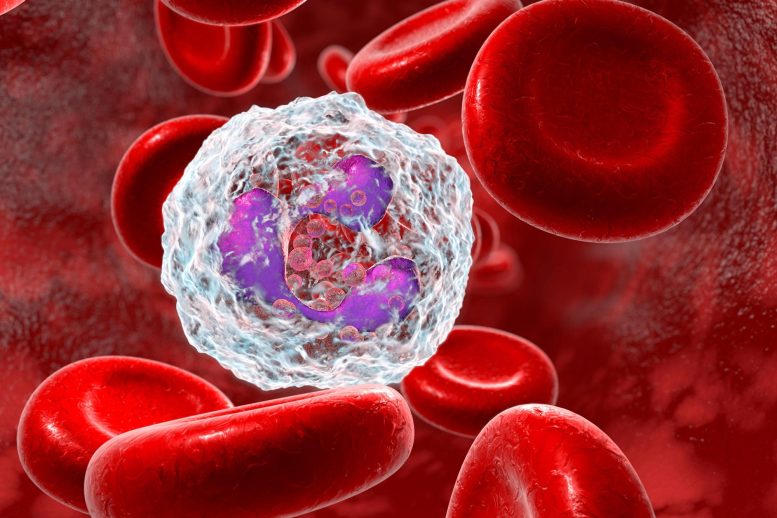
When our bodies become infected, various immune responses are triggered, starting with a release of granulocytes, white blood cells containing special enzymes that makeup about half or more of all human white blood cells.
Neutrophils are also granulocytes that fight off invasive bacteria and fungi, often with zero tolerance for such invaders. Sometimes, however, a balanced and less aggressive approach goes even further in providing a cure.
Now, a team of researchers at Kyoto University has determined that neutrophils induce anti-inflammatory — or M2 — macrophages deep in the core of the granulomas.
In previous studies, chronic inflammatory macrophages were found to have the potential to polarize or differentiate into two opposite versions: pro-inflammatory, or M1, and anti-inflammatory, or M2 types. These constitute an M1-M2 equilibrium that regulates the severity of inflammation and tissue health — or homeostasis.
Granulomas and Microenvironment Manipulation
This dual nature or polarization describes how M2 can revert to M1 or even M0 — the non-inflammatory or steady state — in the deep granuloma zone where a bacteria-permissive microenvironment is formed. The team has examined the dense globular structures of granulomas in animals, particularly in the lungs.
“Microbes and cancer cells may manipulate this permissive microenvironment to favor their survival,” says Tatsuaki Mizutani.
Human granuloma-related disorders including tuberculosis are a hallmark of chronic inflammatory diseases. Mizutani posits that the results his team obtained from tuberculosis may also be applied to tumors.
Previous studies have revealed that intercellular interactions within granulomas drive effective inflammatory responses against pathogens or contaminants, but chronic inflammation — as in tuberculosis and tumors — persists over prolonged periods of time.
To test how to predict tumor development, Mizutani’s team previously established a lung granuloma model in guinea pigs, which demonstrated the specific accumulation of Neutrophil S100A9 — or A9 — deep in the cores of granulomas. A9 is expressed in monocytes and macrophages at low levels but at high levels within neutrophils.
Applications to Cancer Therapy Development
“What is interesting is that both the inflammatory and anti-inflammatory effects of A9 have been reported in A9-deficient mice,” notes Mizutani, whose team is now considering whether to make A9’s multifunctional nature anti-tumorigenic in the tumor microenvironment.
“Our understanding of how a permissive microenvironment in tumors is formed may be applied to effective cancer drug development,” reflects Mizutani.
Reference: “Neutrophil S100A9 supports M2 macrophage niche formation in granulomas” by Tatsuaki Mizutani, Toshiaki Ano, Yuya Yoshioka, Satoshi Mizuta, Keiko Takemoto, Yuki Ouchi, Daisuke Morita, Satsuki Kitano, Hitoshi Miyachi, Tatsuaki Tsuruyama, Nagatoshi Fujiwara and Masahiko Sugita, 29 January 2023, iScience.
DOI: 10.1016/j.isci.2023.106081
Funding: KAKENHI, Ohyama Health Foundation, Fujiwara Memorial Foundation, INFRONT Office of Directors’ Research Grants Program
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.