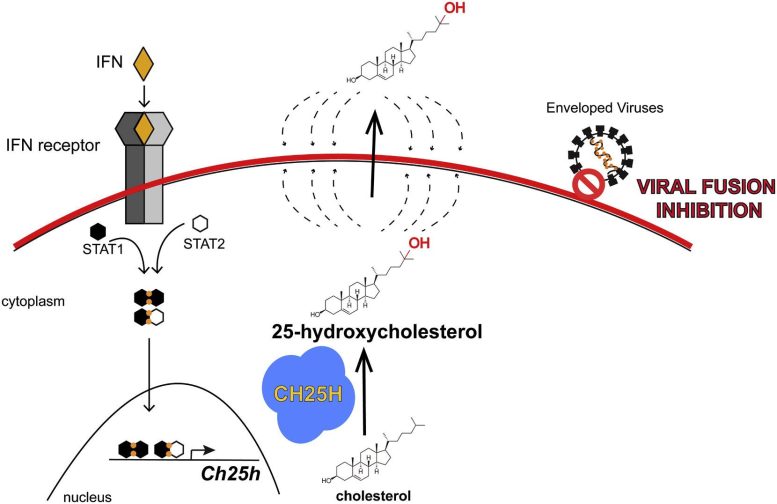
In a newly published study, scientists have shown that an oxysterol called 25-hydroxycholesterol (25HC) suppresses HIV growth in vivo.
A team of researchers led by the University of California, Los Angeles (UCLA) has identified a protein with broad virus-fighting properties that potentially could be used as a weapon against deadly human pathogenic viruses such as HIV, Ebola, Rift Valley Fever, Nipah and others designated “priority pathogens” for national biosecurity purposes by the National Institute of Allergy and Infectious Disease.
In a study published in the January issue of the journal Immunity, the researchers describe the novel antiviral property of the protein, cholesterol-25-hydroxylase (CH25H), an enzyme that converts cholesterol to an oxysterol called 25-hydroxycholesterol (25HC), which can permeate a cell’s wall and block a virus from getting in.
Interestingly, the CH25H enzyme is activated by interferon, an essential antiviral cell-signaling protein produced in the body, said lead author Su-Yang Liu, a student in the department of microbiology, immunology and molecular genetics at the David Geffen School of Medicine at UCLA.
“Antiviral genes have been hard to apply for therapeutic purposes because it is difficult to express genes in cells,” said Liu, who performed the study with principal investigator Genhong Cheng, a professor of microbiology, immunology, and molecular genetics. “CH25H, however, produces a natural, soluble oxysterol that can be synthesized and administered.
“Also, our initial studies showing that 25HC can inhibit HIV growth in vivo should prompt further study into membrane-modifying cholesterols that inhibit viruses,” he added.
The discovery is particularly relevant to efforts to develop broad-spectrum antivirals against an increasing number of emerging viral pathogens, Liu said.
Working with Jerome Zack, a professor of microbiology, immunology, and molecular genetics and an associate director of the UCLA AIDS Institute, the researchers initially found that 25HC dramatically inhibited HIV in cell cultures. Next, they administered 25HC in mice implanted with human tissues and found that it significantly reduced their HIV load within seven days. The 25HC also reversed the T-cell depletion caused by HIV.
By contrast, mice that had the CH25H gene knocked out were more susceptible to a mouse gammaherpes virus, the researchers found.
In collaboration with Dr. Benhur Lee, a professor of pathology and laboratory medicine and a member of the UCLA AIDS Institute, they discovered that 25HC inhibited HIV entry into the cell. Furthermore, in cell cultures, it was found to inhibit the growth of other deadly viruses, such as Ebola, Nipah, and the Rift Valley Fever virus.
Intriguingly, CH25H expression in cells requires interferon. While interferon has been known for more than 60 years to be a critical part of the body’s natural defense mechanism against viruses, the protein itself does not have any antiviral properties. Rather, it triggers the expression of many antiviral genes. While other studies have identified some antiviral genes that are activated by interferon, this research gives the first description of an interferon-induced antiviral oxysterol through the activation of the enzyme CH25H. It provides a link to how interferon can cause inhibition of viral membrane fusion, Liu said.
He noted some weaknesses in the research. For instance, 25HC is difficult to deliver in large doses, and its antiviral effect against Ebola, Nipah and other highly pathogenic viruses have yet to be tested in vivo. Also, the researchers still need to compare 25HC’s antiviral effect against other HIV antivirals.
Reference: “Interferon-Inducible Cholesterol-25-Hydroxylase Broadly Inhibits Viral Entry by Production of 25-Hydroxycholesterol” by Su-Yang Liu, Roghiyh Aliyari, Kelechi Chikere, Guangming Li, Matthew D. Marsden, Jennifer K. Smith, Olivier Pernet, Haitao Guo, Rebecca Nusbaum, Jerome A. Zack, Alexander N. Freiberg, Lishan Su, Benhur Lee and Genhong Cheng, 27 December 2012, Immunity.
DOI: 10.1016/j.immuni.2012.11.005
Additional study co-authors were Roghiyh Aliyari, Kelechi Chikere, Matthew D. Marsden and Olivier Pernet, of UCLA; Jennifer K. Smith, Rebecca Nusbaum and Alexander N. Frieberg, of the University of Texas–Galveston; and Guangming Li, Haitao Guo and Lishan Su, of the University of North Carolina–Chapel Hill.
The National Institutes of Health (grants R01 AI078389, AI069120, AI080432, AI095097, AI077454, AI070010 and AI028697), the Warsaw Fellowship, the UCLA Center for AIDS Research (CFAR), the UCLA AIDS Institute, the UCLA Clinical and Translational Science Institute (CTSI), and the Pacific Southwest Regional Center of Excellence (PSWRCE) for Biodefense and Emerging Infectious Diseases funded this study.
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.