A newly identified weakness in “zombie” cells may open the door to more precise cancer treatments by turning their own survival strategy against them.
A new class of drugs takes advantage of a recently discovered weakness in “zombie-like” or senescent cells, opening the door to potential treatments for cancer and age-related diseases.
Researchers from the MRC Laboratory of Medical Sciences (LMS) and Imperial College London found that these cells exist in a delicate balance. They accumulate high levels of iron and other harmful molecules that push them toward cell death, but survive by producing large amounts of a protective protein.
Disabling this defense removes their protection, making the cells vulnerable. This strategy could be used alongside existing therapies to improve outcomes for cancer patients.
The Double-Edged Role of Senescent Cells in Cancer
Cancer develops through uncontrolled cell division, yet many tumors also contain a subset of cells that no longer divide. These are known as senescent cells. Chemotherapy often increases their numbers as it works to slow tumor growth.
Although these cells do not directly expand the tumor, they still contribute to disease progression. Senescent cells release signaling molecules that affect nearby cells, encouraging tumor growth, spread, and harmful immune responses. They are also linked to age-related conditions such as fibrosis. Because of these effects, scientists are increasingly focused on finding ways to selectively eliminate senescent cells.
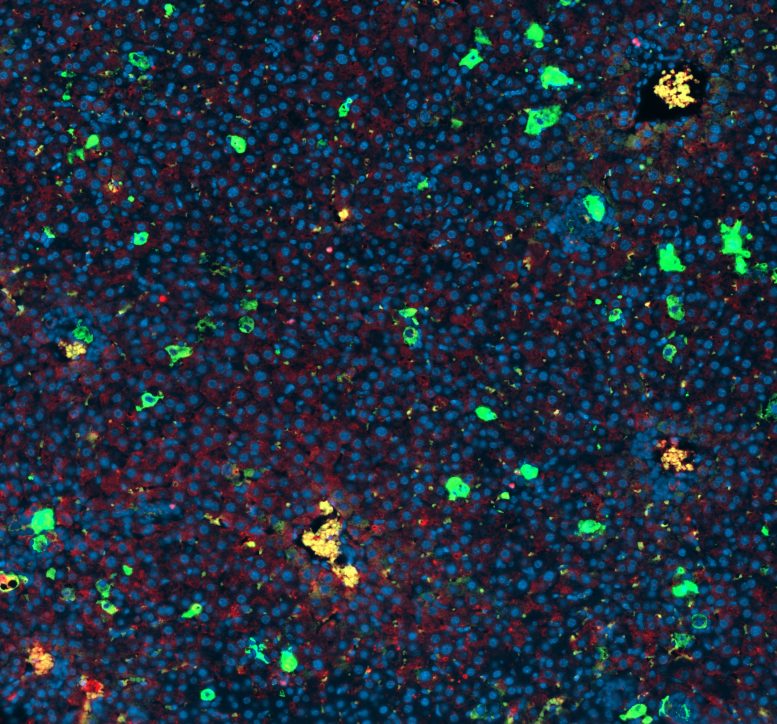
Mariantonietta D’Ambrosio, a postdoctoral researcher at LMS and lead author of the study published in Nature Cell Biology, describes how views on these cells have changed: “Senescence was considered for a long time to be positive, because senescent cells don’t proliferate, which is the core feature of cancer. Normal chemotherapy induces senescence blocking the proliferation of cancer cells, so the tumor doesn’t get bigger. But with time, you also see the negative side of the senescent cells, because they secrete a lot of factors that influence neighbouring cells and induce even more proliferation, metastasis, and recruitment of bad parts of the immune system that will provoke even more aggressiveness in the tumor. For this reason, we tried to find some drugs that were able to kill the senescent cells.”
Testing 10,000 possible drugs
To identify possible treatments, the researchers carried out a large screening effort. Working with collaborators in Imperial’s Department of Medicinal Chemistry, they focused on a group of inhibitors known as “covalent compounds.” These molecules form strong chemical bonds with their targets, allowing them to block proteins that are often difficult to target with traditional drugs.
The team tested 10,000 different compounds on both senescent and normal cells. Their goal was to find compounds that selectively killed senescent cells. Drugs with this property are known as “senolytic,” meaning they specifically eliminate senescent cells.
From this process, four promising candidates emerged. Three of them targeted a protein called GPX4, which plays a key role in protecting cells from damage.
GPX4 helps prevent ferroptosis, a type of cell death triggered by high iron levels and harmful molecules known as reactive oxygen species. Scientists have only recently identified ferroptosis as a vulnerability in senescent cells.
Mariantonietta says, “recent papers have shown this predisposition of senescent cells to ferroptosis, but it’s a new senescence vulnerability. That creates an opportunity for us to exploit. So now there is research to find senolytic drugs to kill cells through ferroptosis.”
Senescent cells accumulate high levels of iron and other damaging factors, which makes them especially prone to ferroptosis. To survive, they produce elevated levels of GPX4. This can be compared to taking a painkiller to keep running on an injured ankle. The underlying damage is still present, but its immediate effects are masked. Removing that protection exposes the full impact of the injury.
When GPX4 is blocked, this protective system fails, and ferroptosis becomes unavoidable. The result is the selective death of senescent cells.
Improved outcomes in three cancer models
The researchers tested these compounds in three mouse models of cancer and observed improved results in each case due to the removal of senescent cells. These findings suggest that targeting such cells could strengthen current cancer treatments.
“In mouse models, we saw that these drugs reduced tumor size, and improved survival. Now we need to see the effect on the immune system. Is the improvement also awakening the ‘good side’ of the immune system (T cells, natural killer cells) that helps to kill the tumor?” says Professor Jesus Gil, senior author and Head of the Senescence group at the LMS. “Once we know more, the next step is to understand which cancer cell types or specific patients might better respond to this treatment. For example, if a patient undergoing chemotherapy overexpressed GPX4 then you could use this approach in combination with existing drugs to improve efficacy.”
This work highlights senescent cells as a promising but underused target in cancer therapy. Mariantonietta adds: “Targeting senescence is a huge opportunity for cancer treatments, and ultimately it can play a supporting role in addition to chemotherapy and immunotherapy.”
Reference: “Electrophilic compound screening identifies GPX4-dependent ferroptosis as a senescence vulnerability” by Mariantonietta D’Ambrosio, Matthew E. H. White, Efthymios S. Gavriil, Laura Bousset, Jodie Birch, Aleksandra Gruevska, Emiliano Pasquini, Manuel Colucci, Winnie Fong, Simone Mosole, Aurora Valdata, Dimitris Veroutis, Katie Tyson, Vikas Ranvir, Sandra Prokosch, Joaquim Pombo, Aoki Ardisson, Sanjay Khadayate, George Young, Alex Montoya, Georgia Roumelioti, Jack Houghton, Jianan Lu, Pavel V. Shliaha, Elena De Vita, Santiago Vernia, Vassilis G. Gorgoulis, Suchira Gallage, Mathias Heikenwälder, Zoe Hall, Andrea Alimonti, Iain A. McNeish, Edward W. Tate and Jesús Gil, 24 April 2026, Nature Cell Biology.
DOI: 10.1038/s41556-026-01921-z
Researchers at several institutions, including the Institute of Oncology Research (IOR) in Bellinzona, Switzerland and the M3 Research Centre at the University of Tübingen in Germany also contributed to this study.
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.
2 Comments
Thank YOU ALL SO MUCH!
SO MUCH IS UNDERSTOOD BETTER BECAUSE SO MUCH IS EXPLAINED BETTER.
PLEASE KEEP US UNDERSTANDING! AS YOU “ALL” LEARN, SHARE AND TEACH US ALL.
I FEEL AS THOUGH “HOPE” IS ON THE WAY!
Well I’m sorry to say I’m not sold by any of this so called groundbreaking research, the reason being that cancers of all kinds are still killing so many ppl, my own father died in 2012 from prostate cancer that the doctors had treated yet returned years later with a vengeance as bone cancer that attacked his spine. Cancer is the 2nd leading cause of death in the US killing one half million Americans of all ages each year. The leading cause of death is heart disease which i see as unavoidable given that unless we make it past 100 and simply die of “old age” like my grandmother did at 107, she just fell asleep one night and didn’t wake up, someday we will all die from some ailment, but why cancer, a fluke where a cell just takes up itself over and over until it takes over our bodies and kills our organs one by one? And after 50 years of research to find a cure spending hundreds of millions of dollars yet to date essentially failing every time, yes if it kills 2000 Americans everyday then no we are not making much progress I’m afraid. So all that positive stuff i just read doesn’t make a hill of beans, it’s just mumbo jumbo designed to keep the funding pouring in. I didn’t use to be this cynical but come on ppl are you really that gullible? I’m sorry to say this but accept the fact as proven by statistics that you or a loved one will probably meet they’re fate at the hands of cancer, a horrible disease that we don’t seem to have any control over