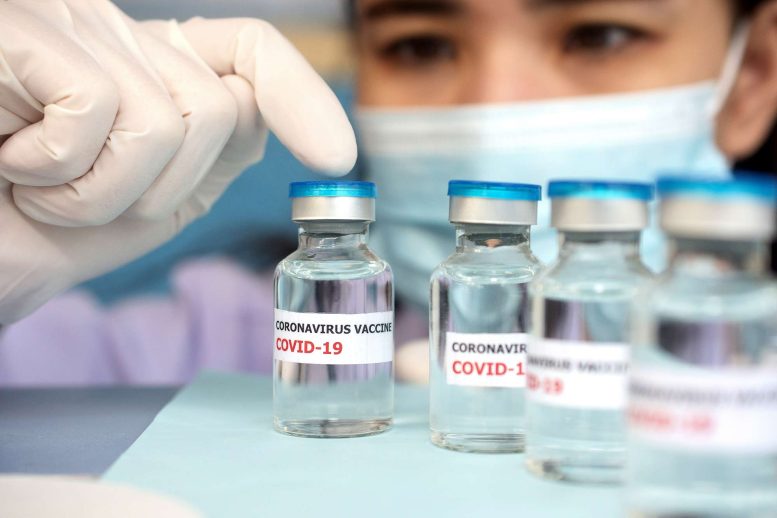
Individuals who have received two doses of COVID-19 vaccine have a reduced, though still notable, risk of contracting the delta variant compared to unvaccinated individuals.
- Study of 621 people in the UK with mild COVID-19 infections found that people who received two vaccine doses could still pass the infection on to vaccinated and unvaccinated household members.
- The analysis found that 25% of vaccinated household contacts tested positive for COVID-19 compared with 38% of unvaccinated household contacts. The infectiousness of vaccinated cases with breakthrough infections was similar to unvaccinated cases.
- Infections in vaccinated people cleared more quickly than those in unvaccinated people, but resulted in a similar peak viral load – when people are most infectious – probably explaining why the delta variant remains able to spread despite vaccination.
- The authors urge unvaccinated people to get vaccinated to protect themselves from severe disease and those eligible for a booster to receive it as soon as offered. They also call for continued public health and social measures to curb transmission, even in vaccinated people.
People who have received two vaccine doses against COVID-19 have a lower, but still appreciable, risk of becoming infected with the delta variant compared with unvaccinated people. Vaccinated people clear the infection more quickly, but the peak viral load among vaccinated people is similar to that seen in unvaccinated people, which may explain why they can still readily pass on the virus in household settings, according to a study published in The Lancet Infectious Diseases.
Vaccines remain highly effective at preventing severe disease and deaths from COVID-19, but some studies suggest they may be less effective against the delta variant – currently the dominant strain worldwide – though the reason for this has not been established. Most COVID-19 transmission is known to occur in households yet there is limited data on the risk of transmission of the delta variant from vaccinated people with asymptomatic or mild infections in the community.
Professor Ajit Lalvani of Imperial College London, UK, who co-led the study, said: “Vaccines are critical to controlling the pandemic, as we know they are very effective at preventing serious illness and death from COVID-19. However, our findings show that vaccination alone is not enough to prevent people from being infected with the delta variant and spreading it in household settings. The ongoing transmission we are seeing between vaccinated people makes it essential for unvaccinated people to get vaccinated to protect themselves from acquiring infection and severe COVID-19, especially as more people will be spending time inside in close proximity during the winter months. We found that susceptibility to infection increased already within a few months after the second vaccine dose—so those eligible for COVID-19 booster shots should get them promptly.”
The new study enrolled 621 participants, identified by the UK contact tracing system, between September 2020 and September 2021. All participants had mild COVID-19 illness or were asymptomatic. Demographic and vaccination status information were collected on enrolment, and participants had daily PCR tests to detect infection, regardless of whether or not they had symptoms. It is one of the few studies to date conducted using such detailed data from real households, offering key insights into how vaccinated people can still be infected with the delta variant and pass it on to others.
In this study, participants were defined as unvaccinated if they had not received a single COVID-19 vaccine dose at least seven days before enrolment, partially vaccinated if they received one dose more than seven days before enrolment, and fully vaccinated if they received two doses more than seven days beforehand. The study took place before vaccine boosters had become widely available.
Risk of transmission based on vaccination status was analyzed for household contacts exposed to delta variant index cases (the first detected case in a household). By performing PCR tests on swab samples provided daily by each participant for 14–20 days, changes over time in viral load – the amount of virus in a person’s nose and throat – were estimated by modeling PCR data, enabling comparisons between fully vaccinated cases of delta infection, and unvaccinated cases of delta, alpha, and pre-alpha infection.
A total of 205 household contacts of delta variant index cases were identified, of whom 53 tested positive for COVID-19. Of the 205 contacts, 126 (62%) received two vaccine doses, 39 (19%) had received one vaccine dose, and 40 (19%) were unvaccinated. Among household contacts who had received two vaccine doses, 25% (31/126 contacts) became infected with the delta variant compared with 38% (15/40) of unvaccinated household contacts.
Among vaccinated contacts infected with the delta variant, the median length of time since vaccination was 101 days, compared with 64 days for uninfected contacts. This suggests that the risk of infection increased within three months of receiving a second vaccine dose, likely due to waning protective immunity. The authors point to vaccine waning as important evidence for all eligible people to receive booster shots.
A total of 133 participants had their daily viral load trajectories analyzed, of whom 49 had pre-alpha and were unvaccinated, 39 had alpha and were unvaccinated, 29 had delta and were fully vaccinated, and 16 had delta and were unvaccinated. Viral load declined more rapidly among vaccinated people infected with the delta variant (0.95 log10 virus copies/mL/day) compared with unvaccinated people with delta (0.79), alpha (0.82), or pre-alpha (0.69). However, the authors note that vaccinated people did not record a lower peak viral load than unvaccinated people, which may explain why the delta variant can still spread despite vaccination as people are most infectious during the peak viral load phase.
Dr. Anika Singanayagam, co-lead author of the study, said, “Understanding the extent to which vaccinated people can pass on the delta variant to others is a public health priority. By carrying out repeated and frequent sampling from contacts of COVID-19 cases, we found that vaccinated people can contract and pass on infection within households, including to vaccinated household members. Our findings provide important insights into the effect of vaccination in the face of new variants, and specifically, why the delta variant is continuing to cause high COVID-19 case numbers around the world, even in countries with high vaccination rates. Continued public health and social measures to curb transmission – such as masking wearing, social distancing, and testing – thus remain important, even in vaccinated individuals.”
The authors acknowledge some limitations to their study. Due to the nature of UK symptoms-based community testing, only contacts of symptomatic index cases were recruited. As this real-world study was undertaken when infection was circulating widely, it cannot be excluded that another household member may already have been infected and transmitted COVID-19 to the index case (resulting in misclassification of who is the index case and who is the contact but this would not affect the conclusion that transmission is occurring between vaccinated individuals). As older age groups were vaccinated earlier during the UK vaccine rollout, the age of unvaccinated people infected with the delta variant was lower than for vaccinated participants, meaning age could be a confounding factor. However, higher transmission in unvaccinated contacts was likely driven by the absence of vaccination rather than younger age as susceptibility to COVID-19 infection does not increase with decreasing age. While the authors did not perform viral culture – a better proxy for infectiousness –two other studies that used the technique reached conclusions consistent with their findings.
Reference: “Community transmission and viral load kinetics of the SARS-CoV-2 delta (B.1.617.2) variant in vaccinated and unvaccinated individuals in the UK: a prospective, longitudinal, cohort study” by Anika Singanayagam, PhD; Seran Hakki, PhD; Jake Dunning, PhD; Kieran J Madon, MSc; Michael A Crone, MBBCh; Aleksandra Koycheva, BSc; Nieves Derqui-Fernandez, MSc; Jack L Barnett, MPhys; Michael G Whitfield, PhD; Robert Varro, MSc; Andre Charlett, PhD; Rhia Kundu, PhD; Joe Fenn, PhD; Jessica Cutajar, BSc; Valerie Quinn, BSc; Emily Conibear, MSc; Prof Wendy Barclay, PhD; Prof Paul S Freemont, PhD; Prof Graham P Taylor, DSc; Shazaad Ahmad, FRCPath; Prof Maria Zambon, FRCPath and Prof Neil M Ferguson, DPhil, 29 October 2021, The Lancet Infectious Diseases.
DOI: 10.1016/S1473-3099(21)00648-4
This study was funded by the National Institute for Health Research. It was conducted by researchers from Imperial College London, University of Oxford, University of Surrey, Public Health England, and Manchester Academic Health Sciences Centre, UK.







Our healthcare system is about to experience a tsunami! Potential side effects of jabs include chronic inflammation, because the vaccine continuously stimulates the immune system to produce antibodies. Other concerns include the possible integration of plasmid DNA into the body’s host genome, resulting in mutations, problems with DNA replication, triggering of autoimmune responses, and activation of cancer-causing genes. Alternative COVID cures exist. Ivermectin is one of them. While Ivermectin is very effective curing COVID symptoms, it has also been shown to eliminate certain cancers. Do not get the poison jab. Get your Ivermectin https://ivmpharmacy.com
Yes, the vaccines are very effective in preventing infection, but even if they’re 95% effective that means 5% of the virus can still infect cells. Our immune system handles low numbers of infected cells adequately, but attacking the spike proteins (as our vaccines do) is only half the story.
All the coronaviruses and all their variants have different protein spikes, with Delta having one that’s more efficient at getting around the vaccines. But the real problem is in the virus itself, not its protein shell, and why the most dangerous (MERS, SARS, and Covid-19) are so infectious. My independent research has found multiple one-in-a-million nucleotide sequence matches between all the coronaviruses and the human genome. Those sequences are the same as some of the loops of human tRNA. Using those loops and their amino acid code matches, viruses may be able to fool the nucleus membrane in cells to allow the virus to enter and associate with the human DNA, creating more opportunities for further infection. Our immune system may be compromised and may no longer be able to stop the virus and other diseases from attacking organs throughout the body. Vaccines that attack the virus protein shells while ignoring their contents are doomed to failure from the Darwin effect, but recognizing these loops suggests a possible approach to successful coronavirus vaccines. Only the infection process is considered in my work, not the innate virulence of the virus. For more info, check out this YouTube, Coronavirus – Using Your DNA Against You. https://www.youtube.com/watch?v=8dOIzD6ch8s
you will die if you have vaccine its proven now by specialists in cardiology, thousands of people dying from heart attacks,just after vaccine
have it if you want but you will die young and old.